LISTS – AND LISTS
I know you are all looking for THE list. Here is one from a reliable source I have have downloaded on my site to a separate document so it opens with one click.
The reliable source, as it turns out, needed some updating. Dr Ross Holmes, professor, School of Medicine, University of Alabama, was kind enough to review the work of Dr. Michael Liebman who is a professor of Human Nutrition and Food Option at University of Wyoming and determine which food entries on the Harvard list needed changing. We cannot change the original but we have updated our lists accordingly and annotated updates with *** marks. So the lists here are the most recently edited available at present.Fred Coe and I have updates and annotated the list for those with a tendency to perfectionism: Updated table of oxalate foods. Set it at 50% for easier reading. Get yourself acquainted with the lists. They will tell you much of what you need to know. A lot of it will even surprise you. You are not as restricted as you think you are or as you have been told.
A more dramatic list is the 177 high oxalate foods we distilled out of the big list. Here are culprits! Not on this list? Probably not very high in oxalate so far as we know – with perhaps a few exceptions. Note that quantity is critical. For example black pepper is high in oxalate but the amounts used are small enough that total oxalate intake from it is negligible.
Eating a low oxalate diet can be overwhelming and difficult to incorporate into your daily life. I just released a course called The Kidney Stone Prevention Course to help you understand how to implement your physician’s prescribed treatment plans.
LET’S DIVIDE AND CONQUER
FOODS TO WORRY ABOUT
A List of Concerning Foods
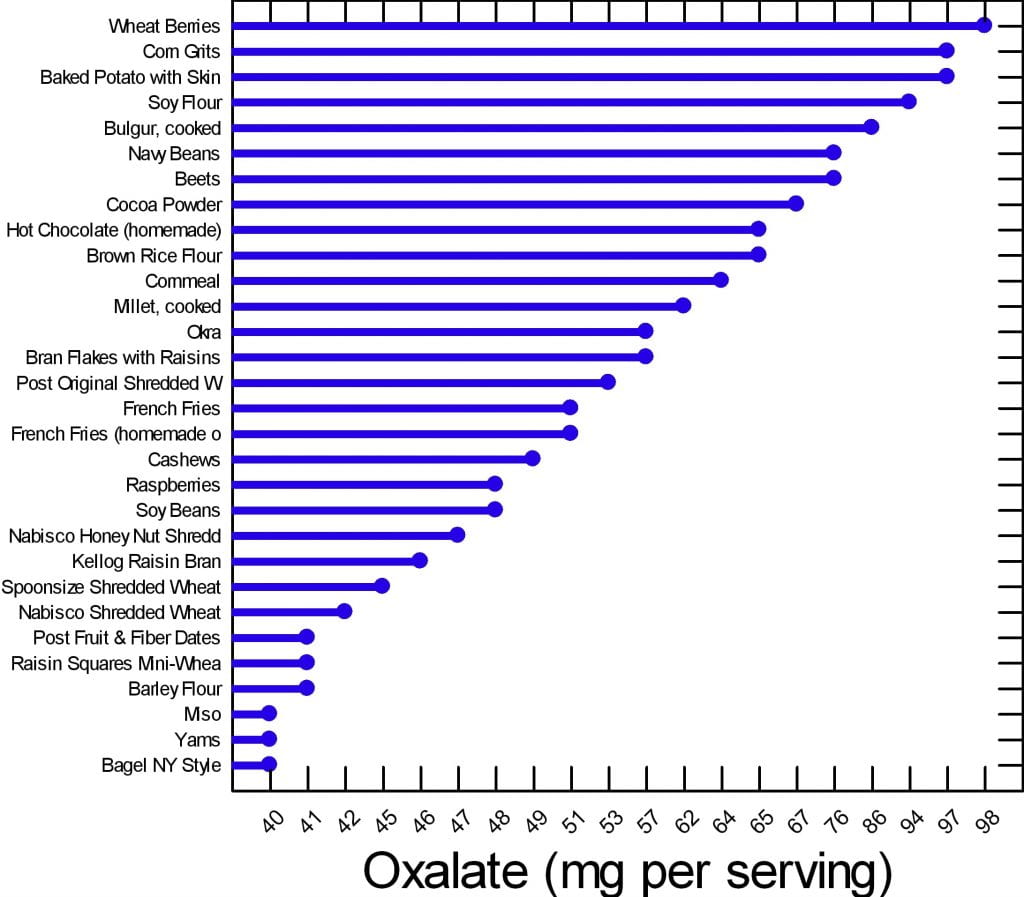
We have created two graphs for this article. Of the 177 foods on our master list, many are of concern but can be used in your diet if you control the portion size and how often you use them. There are 30 of them that are worrisome enough to deserve special attention.
Here are the 30. The graph shows mg of oxalate in a common portion. The details of the portions are in the complete list. The foods have in common that all contain at least 40 mg/serving. All other foods for which we have reliable data have less oxalate per serving.
Your budget is about 100 mg/day.
What does this graph mean? Does it mean you can never have chocolate, or a baked potato?
No.
It means if you want to use your whole budget on a treat, do it, but keep track and make sure you do not overspend in any meal or in any one day. Have your baked potato, but maybe share half with your partner. Or, have some hot chocolate but make it with milk because calcium helps reduce oxalate absorption. Eat your cashew nuts, but pay attention to how many. If one handful leads to ten, you cannot have them.
FOODS TO AVOID
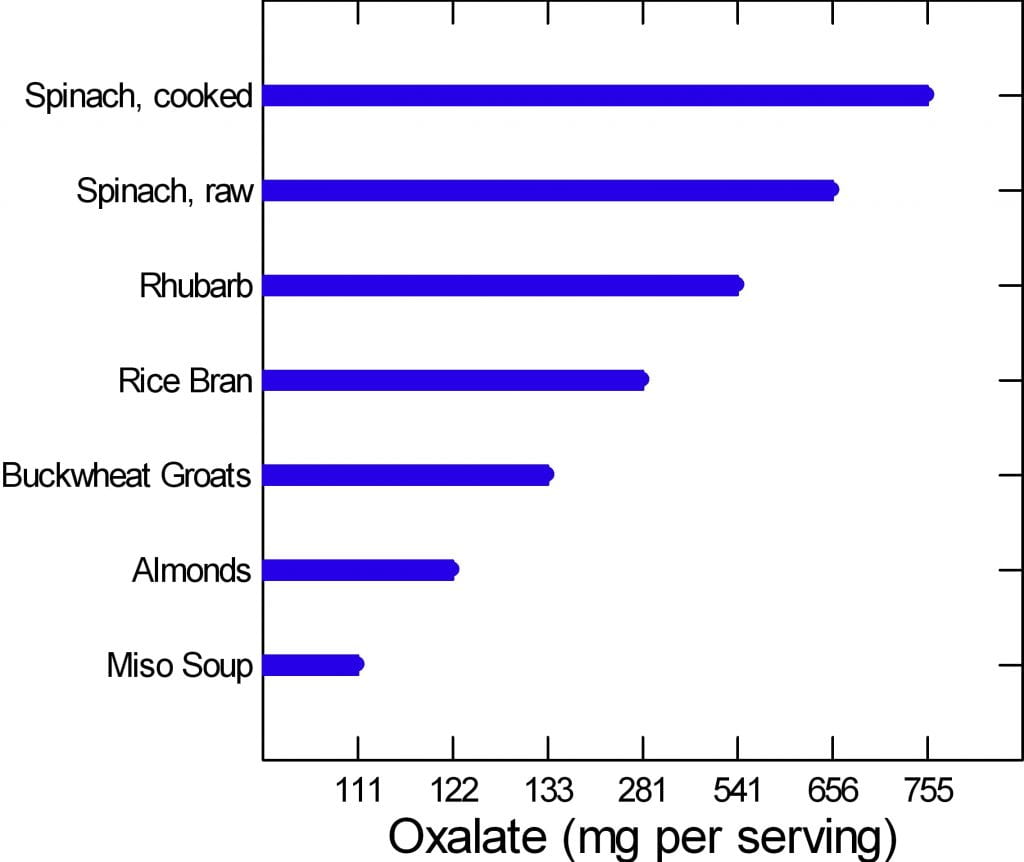 The graph to the left is of the very few dangerously high oxalate foods.
The graph to the left is of the very few dangerously high oxalate foods.
There are only six foods, but spinach, being worst of all, has two entries. Be careful of this plot because of its range. It begins at 100 mg/portion and rises to 755 mg/portion in only 7 steps, so the distance from miso soup to spinach is about a 7 fold increase.
Rhubarb and spinach are so high you just cannot eat them. Rice bran is something few will miss, the same for buckwheat groats.
People like almonds but have a hard time controlling portion size. If you can keep it to 11 almonds a day – the portion size that gives 122 mg of oxalate, alright. Otherwise stay away from them.
If you have to eat any of these foods, caution is hardly a strong enough word.
Are you sure you need to eat them?
Why?
WHAT ARE WE SAYING?
We are saying that oxalate is common in foods, and that you have to be careful, but care is a scarce resource. How much care can you give every bite? The graphs say if you eat moderately high oxalate foods – the first graph – be careful.
Watch portions.
If you are eating one of the six dangerously high oxalate foods, stop eating it.
It is too hard to be careful with those six foods. They have too much oxalate for most of you to handle. So, just say no.
WHY BELIEVE OUR DATA?
These data arose from a major effort at the Harvard School of Public Health. A world class expert has curated it twice. Harvard can be wrong and so can Ross Holmes, but both will tend to be wrong less often than the average persons who attempt to put complex data into the public domain. We have always appreciated comments, and if anyone has a peer reviewed publication with different food oxalate levels than ours, we will read the paper and see if it warrants our making a change.
Medical research is endlessly argumentative, and food oxalate is no exception. A recent paper contrasts findings from 6 websites and 2 applications and finds some wide variations. Of the sites, the Harvard site – used here as our reference, and the Wake Forest site – which is a legacy of an outstanding investigative group have most standing with me. Leaf through the comparisons between them in the 4 charts and in the large table at the very end. On the whole differences are modest. The hyperoxaluria and oxalosis list from the paper has been withdrawn from their site.
DO YOU NEED A LIST?
Sure, a list is nice. But we helping you here. Lists can run on to hundreds of foods. The picture is meant for focus. Here are the ones to focus on.
Many of you leave the doctor’s office thinking you will never be able to eat a fruit or vegetable again. If that wasn’t bad enough chocolate and nuts are gone, too. Some of this sadly is true, most of it is not. I am here to bring you good news: Almost everything, high oxalate or not, can be incorporated into your diet safely.
Do you need a low oxalate diet? You may if your stones contain calcium oxalate crystals and your urine oxalate is high enough to pose risk.
If you do need a low oxalate diet, what is your goal? Less than 100 mg of diet oxalate is good; less than 50 mg is ideal.
If you want to read some of the science about urine oxalate and risk of stones and about how we get to the diet oxalate goals, it is summarized at the end of this article.
Here we assume you do need to lower the oxalate in your diet.
CALCIUM FIRST
Low calcium diets can raise urine oxalate, and the solution may be as simple as a proper calcium intake. There is every reason for stone formers to eat 1000 mg of calcium daily to protect their bones. The common hypercalciuria of calcium stone formers puts bones at special risk when diet calcium is low.
Before changing your whole life around, ask yourself if you are avoiding calcium foods. If so, add them back and ask your doctor to check your urine oxalate again. It may fall enough that a low oxalate diet is not necessary.
If low calcium intake is not your problem, and you need a low oxalate diet, here is my take on how to do it.
WHAT IS THE DIET OXALATE GOAL?
Typical diets contain upward of 200 – 300 mg of oxalate. For stone prevention, a reasonable goal is below 100 mg of oxalate daily. An ideal would be about 50 mg daily if that can be accomplished.
To get there, consider the oxalate contents in common serving portions of all of the foods, and make up a plan for yourself.
FRUITS
FRESH
Everyone who comes to me is very unhappy thinking they can never have a berry again. This is Baloney. The only berry that is very high in oxalate is raspberries (look at the list). On the other hand, people do not realize avocado, oranges, dates, and even grapefruit and kiwi are very high and need caution.
This doesn’t mean you can never have these healthy treats. If you incorporate any of these high oxalate fruits into your morning yogurt you can reduce some of the effects of the oxalate content.
Also look at your portion sizes. You really cannot eat a lot at any one time. Dates are not a good bargain: One date is 24 mg!
CANNED OR DRIED
Canned pineapple is a problem.
Dried fruits have to be a worry because the water is taken out, so a ‘portion’ of dried fruit can be gigantic in oxalate content. Figs, pineapple and prunes are standouts. Just think: 1/2 cup of dried pineapple is 30 mg – not a lot of fruit for a lot of oxalate. If you want dried fruit, think about apples, apricots, and cranberry as lower oxalate options.
VEGETABLES
Spinach and rhubarb are standouts; stay away.
Other vegetables you need to be aware of are tomato sauce, turnips, okra, and yams (sweet potatoes) along with beans of different sorts.
I am not in the business of taking healthy foods away from people. But in the cases above you really must limit; there is just too much oxalate and these foods do not pair well with high calcium foods the way fruits can be mixed right into your yogurt or cereal and milk.
Many of you have been told to stay away from all green leafy vegetables. This is not true. Look at the list. There are plenty of salad options still available for you including kale. Even though tomato sauce is high in oxalate (see below) that is because of concentration. A whole medium tomato is only 7 mg and who eats more than one at a time?
Many of the salad vegetables are so low in oxalate they are freebies. Eat what you want.
POTATOES
These are Trouble! I put them into their own separate group even though they are vegetables.
From french fries to baked potatoes they are very high oxalate items. One ounce of potato chips has 21 mg of oxalate and who eats one ounce? Not I. Baked potatoes are terrible. One comes in at just under 100 mg of oxalate. Mixing sour cream into the potato will not help much; one tablespoon of sour cream contains only 14 mg of calcium. One ounce of cheddar cheese contains 200 mg of calcium, which could help, but it increases calories, salt and fat. But all in all, why struggle so hard? Potatoes are not ideal for stone formers.
DAIRY PRODUCTS
They have no oxalate. They are your main source of calcium. Use them. They can add a lot of salt – cheeses – and can be caloric. But they reduce oxalate absorption and preserve your bones.
For a stone former who has to watch salt intake, increase calcium intake, and lower oxalate intake, here is how to do that. You cannot have as much cheese as you want because of the salt. So portion sizes are very important. Yogurt, milk, even ice cream are good bargains – modest sodium and high calcium. These are a great place to add in a wee bit of chocolate – high oxalate foods – for those of you who cannot live without these high oxalate treats.
BREADS AND GRAINS
Some of the basic ingredients to make these foods are very high. White flour and brown rice flour are high in oxalate so everything you make from them will be high.
BREADS
Even so, as far as kidney stones go, breads are mainly alright because of portion size: not that much flour so one slice is 5-8 mg. French toast and New York style bagels top the list at 13 mg for two slices and 40 mg for one bagel – as much as anyone will eat of either food.
PASTA RICE AND GRAINS
Spaghetti, one cup cooked is 11 mg and most of us eat more than one cup.
Buckwheat groats, one cup cooked is 133 mg – I don’t see many of you saying ‘darn it’ or taking to your bed, but beware. Millet and bulger, wheat berries, rice bran, corn grits, and corn meal, these are widely used and are high. If you are using these, be thoughtful.
Here are some low oxalate options in this category: White rice, hummus, corn flour, corn bran, flax seed, and oat bran are popular and safe.
MEAT PRODUCTS
Since oxalate is only found in plant foods, all the meats are safe. Fish, too.
For our vegetarian friends, tofu and veggie burgers are very high.
NUTS AND SEEDS
These are just dangerous for two reasons.
Obviously they are very high in oxalate.
Secondly, I don’t know anybody who just has a few nuts at a time.
Just like chips no one eats one – the whole jar is more like it.
But, for one cup of pumpkin sunflower or flax seeds the highest is only 17 mg of oxalate and none for flax. For those of you who love foods in this category seeds are the better choice and they can be sprinkled on yogurt and ice cream.
SWEET STUFF
I have good news for my chocolate lovers. I know most of you have been sent home with a list and chocolate is high on it. But if you look at the numbers nuts are a lot worse than chocolate. Chocolate can be mixed in with dairy products, too, so as to reduce oxalate absorption.
Even so I do want to point out that half a brownie is on the high side, and who eats one half?
You can still satisfy your sugar craving but pay attention to your portion size.
Keep in mind, however, that sugar loads increase urine calcium loss which increases stone risk, so there are two reasons why this food group can be a problem.
But even without chocolate, you eat a lot of flour when you eat a piece of cake, so cake can be a problem – about 15 mg per piece, like french toast. Pies are half the risk because of their fillings – unless they are chocolate pies!
CRACKERS AND CHIPS
The big enemy here is potato chips. A one ounce serving contains a whopping 21 mg of oxalate. I repeat: A one ounce serving.
Your best bet in this category if you’re looking for something crunchy is corn chips – one ounce is 7 mg, popcorn – one cup is 5 mg, and pretzels, one ounce is 5 mg.
Crackers are OK mainly because they are small and the amount of flour is not that much.
BEVERAGES
PLANT SOURCES
Hot chocolate is the clear loser at 65 mg per cup; carrot juice is the runner up at 27 mg per one cup. Lemonade, tea, tomato juices, rice dream and the like are better but still high. The are 15 – 18 mg per serving. Lemonade – frozen concentrate – is 16 mg per 8 ounces so be careful about this as a source of citrate.
Soy milk, for those of you who prefer it, is not a good option. It is very high at 20 mg per cup. We have no data from standard sources for rice milk, cashew milk, and coconut milk; almonds are high in oxalate so the almond milk product will certainly be high.
Tea is so commonly used, here are the details. If you brew your own tea it is high in oxalate. The longer you steep your tea, the more oxalate it will have in it. If you use a sweetened instant iced tea one cup has 0 mg of oxalate.
Here are some juices that are low in oxalate and better substitutes: Apple juice, apricot juice, orange juice, grapefruit juice, grape juice. For all the lemonade drinkers, diet lemonade is low in oxalate.
Here is something very important: Coffee is oxalate free – almost, 1 mg for a cup (2 mg/cup for decaf). We already told you that coffee drinkers have a reduced stone risk, so lets debunk the coffee myth here: Drink it as you wish.
DAIRY SOURCES
Everything is good except chocolate milk. Even that is only 7 mg a cup for a sweet treat here and there.
ALCOHOL
What tops the list in this category is a can of beer: 4 mg of oxalate. All the rest are low and, frankly, the oxalate in a can of beer comes with a lot of fluid. This is not the problem area for stone formers.
WATER
If I didn’t say this to you I could not sleep well tonight. Water is the clear winner in this whole category. It is free of calories, sugar, and oxalate. Please use it as your main beverage and supplement with the items above.
SPREADS AND SAUCES
Chocolate, miso, peanut butter, and tahini are all high.
SOUPS
Miso soups is extremely high – 111 mg/cup. Lentil soup is high, and so is clam chowder – the potatoes.
BREAKFAST FOODS
This is a dangerous meal if you are a cereal lover. Many cereals are high in oxalate. I am afraid you need to look them up in the list by brand. Unfortunately the healthier cereals are highest in oxalate because they contain more plant based ingredients. Probably having milk in your cereal is wise, but we have no data to show.
Eating a low oxalate diet can be overwhelming and difficult to incorporate into your daily life. I just released a course called The Kidney Stone Prevention Course to help you understand how to implement your physician’s prescribed treatment plans.
HOW DO WE MANAGE ALL THIS?
The first thing you need to do is to learn and remember what are the highest oxalate foods and beverages. Without this in mind it is impossible to shop and cook intelligently. Here is a short list of the highest oxalate foods all in one place.
BREAKFAST
For those of you who love cereal because it is quick and easy check out the list and see if the one you love is high in oxalate. If it is, choose the next best one with lower oxalate. Put milk in the cereal.
Alternatives to cereal that are also quick and easy: Yogurt or cottage cheese and fruit. The only fruits to worry about are raspberries because no one puts oranges on their yogurt. Bananas, peaches, blueberries and strawberries are perfect toppings.
More trouble, but no oxalate, eggs any way at all. Boil a batch on Sunday and have them for the week for breakfast, and snacks, too.
Your breakfast coffee is free and so is your water. For juices use orange, apple, pineapple, grapefruit – all great. If you want tea, don’t steep more than a minute and consider adding milk to it. Green tea is better than black.
LUNCH
Typically you are grabbing a salad or a sandwich for lunch, so what now? Many clients tell me they no longer eat salads because their physicians told them to stop all green leafy vegetables.
I’m bringing salads back to you.
Arugula, iceberg, romaine lettuces, and kale, are fine as your base. Stay away from spinach. Here are good toppings. Cauliflower, corn, cucumber, mushrooms, onions, peas, scallions, squash and zucchini are all fine. Tomatoes are fine, too; it is only the sauce that is high. Broccoli and green pepper are moderately high so watch the portion size.
Sandwiches will cost you between 12 and 16 mg of oxalate depending on the bread you are using – 2 slices. This doesn’t mean you can never have a sandwich, it just means you have to keep track of how much. You can have 50 to 100 mg daily. What goes inside between the two slices of bread is usually cheeses and meats which are oxalate free. So sandwiches are not something to be afraid of.
SUPPER
Beef, chicken and fish are all fine, and those the main courses for most of us. You will run into problems if you are a pasta or potato eater. If you are you need to limit the amount of times you have these foods each week and also the quantity each time you use them. Substitutes are a problem: White rice is a nice substitute for potatoes but there are few others. It is more veggies that have to fill in – very healthy but not as much fun.
Here is a recipe for cauliflower – ‘mashed potatoes’ you will like and even think, sometimes, is the real thing. There are many versions on the web, choose the one that makes you happy but be careful about the ingredients.
There is also quinoa which is not on our lists, but may well be high. A recent scientific article on this plant does not give oxalate contents which suggests they are not reliably known.
I have recently put together a private FB page called THE Kidney Stone Diet. It is a group that helps educate you on your physician prescribed treatment plans. As you can imagine, oxalate comes up in many posts. I moderate it to keep it clinically sound. Come on over and join the discussion!
URINE OXALATE AND RISK OF KIDNEY STONES
I promised you some science – here it is for those interested. It concerns only highlights from the food – urine oxalate research recently performed and seemingly germane to the problem of how stone formers should control oxalate intake.
The most useful data about urine oxalate we have so far is from three cohorts studied by Dr. Gary Curhan. Two are cohorts of nurses one a cohort of physicians. These people have kept track of many aspects of diet and health for decades, and among their records are onset of kidney stones.
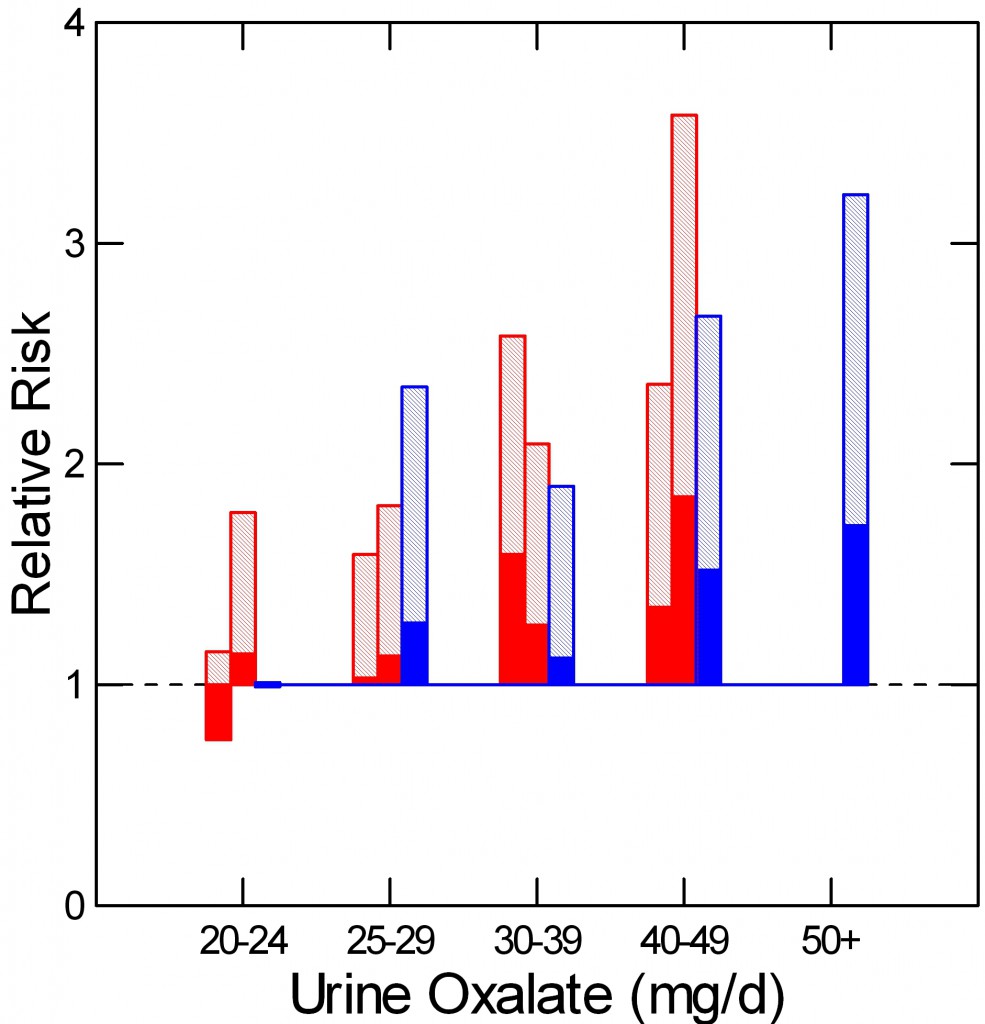 As he did for urine calcium, Curhan measured urine oxalate in properly selected subgroups from each cohort, including people who did and did not begin forming stones. From these samples he could calculate the relative risk of new onset of stones in relation to 24 hour urine oxalate excretion.
As he did for urine calcium, Curhan measured urine oxalate in properly selected subgroups from each cohort, including people who did and did not begin forming stones. From these samples he could calculate the relative risk of new onset of stones in relation to 24 hour urine oxalate excretion.
The two nurse cohorts are red, the physicians – all men – are blue. The dotted line at 1 is the risk threshold: Above that line, risk is present.
The top of each crosshatched bar shows the mean relative risk for each of the five urine oxalate ranges. Clearly the mean goes up as urine oxalate goes up.
But the mean relative risk has a range of uncertainty around it. The bottom of the solid portion of each bar is the lower 95th percentile for that range of uncertainty. When that bottom lies above 1, risk is very likely to be present.
For both the women and men groups, that point is reached between 25 and 30 mg of urine oxalate a day. Therefore one wants to try to get urine oxalate below 30 mg daily and even lower, below 25 mg daily if possible. The average urine oxalate excretion among the women in this study was close – 26 and 28 mg/day for those who did not form stones and just a bit higher for those who did – 28 and 30 mg per day. The men are a problem: 39 and 41 mg/day for those who did not and those who did form stones.
This is not diet oxalate, it is urine oxalate. Urine oxalate is how much the body makes and how much is absorbed from foods. Mostly, we can control only the second part – how much is in the food.
HOW MUCH DIET OXALATE DAILY
All dietary advice depends on having a reasonable goal in mind for oxalate intake. My goal of 50 – 100 mg of oxalate from food daily is not unreasonable given the research that has been done in normal people and stone formers.
Holmes and colleagues found a urine excretion of oxalate of about 10 mg/gm urine creatinine in normal 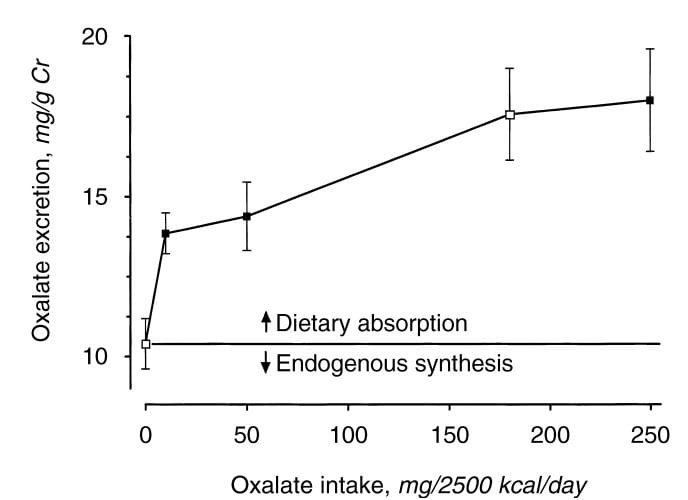 people eating a synthetic oxalate free high calcium diet (graph at left). As diet oxalate increased, urine oxalate rose from 0 to 10 mg/2500 kcal/d, urine oxalate rose steeply from 10 to 14 mg/gm urine creatinine. It rose more slowly, from 14 to barely 15 mg/gm urine creatinine as diet oxalate was increased to 50 mg/2500 kcal/d, and more or less at the same slope thereafter so that an increase from 50 mg/2500 kcal/d up to 250 mg/2500 kcal/d increased urine oxalate only from 14 to 18. The closed symbols are whole food the open symbols synthetic diets.
people eating a synthetic oxalate free high calcium diet (graph at left). As diet oxalate increased, urine oxalate rose from 0 to 10 mg/2500 kcal/d, urine oxalate rose steeply from 10 to 14 mg/gm urine creatinine. It rose more slowly, from 14 to barely 15 mg/gm urine creatinine as diet oxalate was increased to 50 mg/2500 kcal/d, and more or less at the same slope thereafter so that an increase from 50 mg/2500 kcal/d up to 250 mg/2500 kcal/d increased urine oxalate only from 14 to 18. The closed symbols are whole food the open symbols synthetic diets.
From this work the percent oxalate absorption could be calculated as around 10 – 15% and the contribution of diet oxalate to urine oxalate excretion as around 25 – 40% when intake of oxalate was between 50 and 350 mg/2500 kcal. Therefore one can consider a whole food 1000 mg calcium 50 mg oxalate as a usable low oxalate diet, and a 150 – 250 mg oxalate diet as relatively high.
The balance between diet calcium and diet oxalate does not matter greatly if diet calcium is high. Among normal men and women eating 1000 mg/day of calcium and 750 mg/day of food oxalate, 24 hour urine calcium was about 110 mg/day and oxalate about 44 mg/day.
If the calcium oxalate balance is altered so calcium intake is 400 mg and 20 mg of oxalate at breakfast and lunch, and 200 mg of calcium and 710 mg of oxalate at dinner, as compared with simply 333 mg of calcium and 250 mg of oxalate in all 3 daily meals, urine oxalate is lower after the high calcium low oxalate meals, but only slightly higher after the high oxalate low calcium evening meal than when calcium and oxalate intakes were balanced. This means that when diet calcium is at least 1000 mg daily the balance of calcium to oxalate within any one meal is not likely to affect stone risk.
Seiner and colleagues make clear that stone formers are different from normal people. They divided male and female stone formers into 2 groups of 93 people each, one with urine oxalate above 0.5 mmol (~50 mg) of urine oxalate daily and the other with urine oxalate below 0.4 mmol (~40 mg) daily. They found virtually identical calcium and oxalate intakes: 845 vs. 812 calcium and 101 vs. 130 mg daily of oxalate respectively in the lower and higher urine oxalate groups. But the below 0.4 mmol group excreted only 27 mg of oxalate daily on average, whereas the high oxalate group excreted 64 mg daily. In other words diet was not responsible for the higher urine oxalate excretion, suggesting a difference of oxalate absorption. Those prone to high oxalate excretion seem, therefore, to most need diet modification.
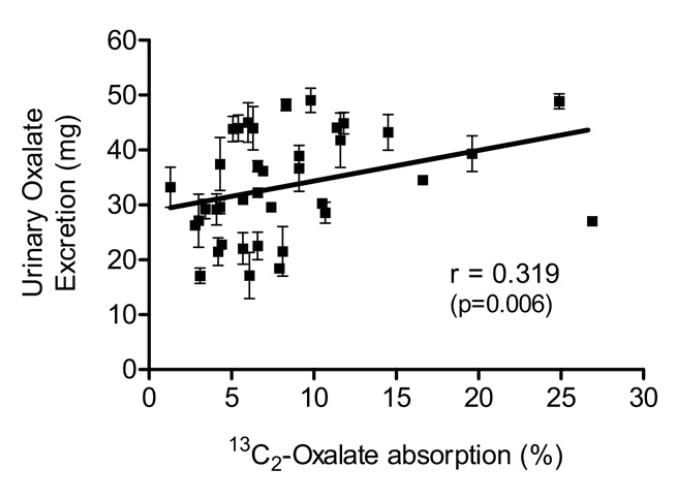 Knight and colleagues found a wide range of oxalate absorption among 38 calcium oxalate stone formers eating a self choice diet. Urine oxalate excretion (vertical axis) varied with percent of diet oxalate absorbed (horizontal axis). The mean absorption centered around 5%; a few outliers absorbed over 15% up to 25%. This supports what Seiner found – some stone formers will have urine oxalate levels very responsive to diet oxalate and sans a research protocol we will not know. This is another good reason to keep diet oxalate low – 50 to 100 mg if possible.
Knight and colleagues found a wide range of oxalate absorption among 38 calcium oxalate stone formers eating a self choice diet. Urine oxalate excretion (vertical axis) varied with percent of diet oxalate absorbed (horizontal axis). The mean absorption centered around 5%; a few outliers absorbed over 15% up to 25%. This supports what Seiner found – some stone formers will have urine oxalate levels very responsive to diet oxalate and sans a research protocol we will not know. This is another good reason to keep diet oxalate low – 50 to 100 mg if possible.
PROTEIN AND GELATIN
Diet protein intake does not affect urine oxalate excretion. In 11 normal people fed a 1000 mg calcium, 51 mg oxalate, 3000 mg sodium fixed diet, varying protein intake from 0.6 to 1.6 gm/kg/day – a very wide range – did not alter urine oxalate appreciably (mean values were 23, 23, and 25 mg daily for the three protein intakes) even though oxalate precursors like glycolate rose markedly (25, 22, and 46, mg daily).
Jello is a source of hydroxyproline which converts to glycolate and oxalate, and oral loading with gelatin can raise urine oxalate. Ten normal people eating a 1000 mg calcium, 150 mg oxalate diet (typical normal level) were fed supplemental gelatin as one quarter of daily protein intake. Urine oxalate was 24 mg daily vs. 17 mg daily when the same diet was supplemented with whey protein – containing little hydroxyproline – as a control. So lots of jello is not an ideal plan for stone formers.
Where does this leave us about how much oxalate is alright for a day. If diet calcium is high, as it should be, at about 1000 mg, then one should try to limit diet oxalate below 100 mg daily. Perhaps this is most important in those patients whose baseline oxalate excretions are higher – in the range of above 40 mg daily.
Eating a low oxalate diet can be overwhelming and difficult to incorporate into your daily life.
For those who need special help, I run an online course: The Kidney Stone Prevention Course to help you understand how to implement your physician’s prescribed treatment plans.



I have one kidney stones in my uterus so I’m trying to be proactive
Hi Careen, I presume you mean the stone is in your ureter. Of highest importance is whether it is causing obstruction of the kidney. If so your urologist needs to keep close track to protect the kidney from damage. As for having a stone, I would suggest a proper evaluation for cause. Diet oxalate is not usually a main issue, and I would not concern myself until you knew if your urine oxalate were indeed high. Regards Fred Coe
Sir I have two stone of 14mm and 10 mm in left kidney attached to mid pole and lower pole of kidney respectively
Hi Laxmi, Get them analysed when removed or passed. If possible get evaluated for prevention. Best, Fred Coe
I just started reading “Toxic Superfoods” by Sally Norton. She explains high oxylate foods contributes to many conditions even kidney function challenges and other neuro degenerative conditions. The list of health challenges with high oxylate diets seems ever expanding. I have large gallstones and oxylate crystals form thise as well apparently. My sister-in-law has severe kidney disease. According to Norton, high oxylate diets can be direcly coorelated. My sister has pulmonary fibrosis. I found a study showing oxylate crystals were found in lung tissue of PF patients.
I am hoping the university can expound on the other correlatedhealth challenges with high oxylate diet so the public can start understanding, a low oxylate diet should not be limited to people with jidney stone issues, but should be universally embraced as a healthy eating plan for disease prevention.
Hi (I cannot decode your name); In chronic kidney disease oxalate can play a role causing progression – in some studies one has such data. In people with normal kidney function I am more than sceptical that food oxalate – as opposed to toxic doses – can have any effects. Our own measurements over several decades place serum oxalate at about 2 – 4 um and plasma calcium oxalate saturation well below 0.1. Formation of calcium oxalate crystals in lung are not known apart from chronic kidney disease. When kidney function is impaired food oxalate can matter, with normal kidneys I cannot accept the idea unless new and convincing data are published. Best, Fred Coe
Hi
Hi Dr. Coe,
I’d likento eat almonds and chia seeds to lower LDL cholesterol. Is it possible to eat these together and use a calcium supplement to offset the oxalate?
Hi David, I presume you are a stone former. I would use some calcium containing food as opposed to calcium supplements. For example, some yogurt, or a small glass of milk. Best, Fred Coe
There is so much contradiction all over the internet it’s very discouraging. I was just in the ER for a first-time kidney stone (4mm) and the most excruciating pain that I never want to repeat. One site tells you no grapefruit (not a problem, don’t like) and another one tells you it’s okay. White potatoes, yes. White potatoes, no. Blueberries are high. No blueberries are low.
Take a look at this list for yourself and see where the contradictions are.
https://www.nephrologyonline.com/wp-content/uploads/2023/01/Low_Oxalate_Diet.pdf
Frankly, the medical community needs to get their s*** together.
Hi T, While diet oxalate seems as if it was the most crucial and the first thing to consider, that probably is not the case most of the time. Here is a reasonable view of how to get evaluated for cause of your stone(s). That is an essential, and very often urine oxalate will not be of importance. Take a look and if you agree get the evaluation and then plan your prevention accordingly. Regards, Fred Coe
Since having a kidney stone a year ago and having it removed and being on a low 50 mg oxalate diet, I have lost considerable weight, down to 100 pounds. I’m 5 ft 2 inches 72 year old woman. How do I GAIN weight?
Hi Mary, I recommend consulting with an expert on diet for kidney stone prevention who can help you maintain weight and control oxalate. Jill Harris is very expert. Regards, Fred Coe
Hello, Doctor.
Quick question: (regarding the “HOW MUCH DIET OXALATE DAILY”) why be so restrictive to 50-100mg recommendation when you could go to 250mg without significant increase in excretion (from 15mg to 17mg…) and being that increase still well bellow the before mentioned cutoff risk of 30-40mg? Best regards
Hi Oliveira, I am not clear as to your source for urine oxalate changing between 15 – 17 mg/d when diet oxalate changes from 100 to 250 mg/d. Can you help here? It is true that with high calcium diet, and especially in non stone formers urine calcium is not as highly related to diet oxalate but your figures are at an extreme. A reference would be appreciated. Regards, Fred
I need meal plan for my 1 cm kidney stone
Hi Marina. Here is my best on it. Be sure and analyse the stone. Regards, Fred
Why no mention vitamin B6 and probiotics as treatment?
Hi Vin B, Because I know of no reliable data showing either prevents stones. They are well spoken about remedies lacking evidence. Regards, Fred Coe
Being a former NY’er, I love my bagels.
The Harvard oxalate list says a NY bagel has 40mg and a plain bagel has 9mg.
Can someone advise me what a NY bagel consists of to give it 31 more mg of oxalates?
Hi Frank,
Most likely because of the giant size of NY bagels. Other than this I can’t think of anything. But of course you can still eat your beloved bagel. This is a portion game.
Jill
I assume it is the sesame seeds – if they are used. They are extremely high in oxalates.
Hello Jill, When we make a vegetable soup (organic potatoes, organic carrots, organic white cabbage, onions), we now take half the vegetables, drain the broth, and add them to a bowl with fish broth. The question is, can the vegetables that are left overnight in the original vegetable broth (for the next day’s meal) reabsorb the oxalates now boiled out and contained in the broth? Thank you in advance for your answer. A.T. in B.C., Canada.
Why does nobody mention arrow root flour for a low oxalate alternative to wheat and corn flour?
Hi Bethankit,
Arrowroot has been on high and lower lists so we are not sure where it stands. That being said one whole cup of wheat flour has 29 mg of oxalate and foods that contain whole wheat are typically not in portions of one cup. So ww flour can surely be eaten. The oxalate portion of the kidney stone diet is all about portion size. Most foods can safely be eaten on a lower oxalate diet once you take away eating the highest oxalate foods in large amounts.
Jill
The Harvard list shows a regular bagel vs a NY bagel. Does someone know what the different is, seeing as a NY bagel has 4 times the amount of oxalate?
Hi Frank,
The huge size of the NY bagel
Nurse Jill
What about chamomile tea? Does it contain high levels of oxalate?
Hi Sarah,
Potatoes are on the higher side so the starch most likely would be as well. Go to my website for everything oxalate. kidneystonediet.com/oxalate-list
Nurse Jill
Thank you for this great article. You simplified a complex issue and made very useful recommendations.
What do you think about the Peruvian herb, Chanca Piedra. There are some studies that have shown benefit.
Hi CM, Chanca is an unproved remedy with a sketchy background and much hype. I should do an article about it but have not had sufficient interest to make that happen. I doubt it has any merit but that is not any kind of proof. Fred
Hello!
I am a recurrent stone former with nephrocalcinosis, medullary sponge kidney, and multiple cysts therein. I have terrible GI issues whenever I take potassium citrate, so I lose more water than I drink to replenish it. My urine is not alkaline enough to prevent stones, and the 2 10 meQ pills a day were helping with those levels, despite the GI issues that made everything so much worse.
Do you have any suggestions for an alternative to potassium citrate? I’m just trying to work on stone prevention first, and then possibly dissolving a few next. I am seeing a handful of specialists for this that are stumped by my condition.
Thank you!
Hi Elise, you pose many problems for me. What are your stones made of? Usually an increase of pH is to prevent uric acid stones. Do you have 24 hour urine results? Right now I just cannot say anything worthwhile sans more information. Regards, Fred Coe
Great web site you have here. It’s hard to find high-quality writing like yours these days. Thank you for your articles. I find them very helpful. I really appreciate people like you! Take care and have a great day ahead!!
Karya Bintang Abadi
Hi Karya, Thank you for noticing. Fred
Your site is very informative and also warm and friendly. Been low oxalate for 3 years after discovering Sally K Norton. Surprised you do not mention her and her extensive work.
Hi, Thanks for mentioning. Fred
I realized licorice isn’t anywhere on the lists, and a “quick” search found another article suggesting that Licorice root also has a lot of oxalate in it (“Licorice root is also one of the highest oxalate-containing foods. (3569.3 mg/100 g)” – https://jmedicalcasereports.biomedcentral.com/articles/10.1186/s13256-023-04129-z#:~:text=It%20is%20well%20known%20that,100%20g)%20%5B13%5D.)
My real question is how that number (3569.3 mg/100 g) relates to this study. If I’m doing my math correct, this would break down to 127.46mg / ounce, which does seem like a lot, so wondering why its not on the list at all.
Also, can’t find any information on Red licorice, which is something I thought was an okay snack before but now I guess it would be nice to know.
Thanks for any response.
Hi Michael.
I would be more concerned with sugar than oxalate. Eat licorice as a here and there food. How much licorice root would actually be used in the candy? Portion matters.
Nurse Jill
I have had stones for 10 years. I started with a new urologist and he is younger and more aggressive. I had 3 procedures over 3 weeks, 4 ureter stents. 10-12 stones removed, including my 4th obstructing stone.
I have a hx of IBS and for the past 5 years my IBS diet has made/fed these stones.
I’m trying to reintroduce dairy to my diet and completely change my eating habits as my safe foods were potatoes, pasta, spinach salad, veggie and impossible burgers.
Any suggestions of a balance to manage both IBS and chronic kidney stones?
Sincerely
Tiaya Welsh…. Aka long time stoner.
Hi Tiaya, The main issues for stone prevention are reduced diet sodium, adequate food calcium, and reasonable attention to food oxalate. Monitoring with 24 hour urines is critical to assure things went as planned. Reduced sodium should pose no GI issues. For calcium, milk is ideal but yogurts of all kinds work very well. But for details, I advise using my partner’s program that gives far more diet information. Regards, Fred Coe
My husband and I are vegans. You say you think quinoa is high in oxalates. It looks like almost everything we eat to get protein is on the high oxalate list. What do you suggest as a low oxalate diet for vegans?
hi Mimi,
So much from my website on vegans and oxalate.
kidneystonediet.com/blog
Nurse, Jill
What about chamomile tea? Any oxalates in it?
Any info about pumpkin butter? I assume it would be lower in oxalates than peanut or almond.
Thanks:)
Hi Jason,
Find out about the foods Harvard didn’t study from this oxalate page from my website: kidneystonediet.com/oxalate-list
Nurse Jill
Hello,
I am maintaining a food plan based on weighing and measuring all the foods I eat. I have a concern about how much protein and calcium I consume. Currently on my food plan is a total daily intake of 6 oz protein (mostly animal and some beans), 2 oz of cheese and 8 oz yogurt. Per your Kidney Stone diet, you recommend 1200 mg/day (I am postmenopausal) and .8-1 gm/kg/day for meat. Is my current food plan too much for your recommendations? Is there any adjustments I need to make…also when I weigh my food, I use ounces rather than gm/kg.
Hi Rho,
Go to this article to figure out total protein for you.
Nurse, Jill
I forgot to mention I also eat butter as a fat, and I consume 2 tbsps of butter daily with my lunch and dinner meals.
My latest 24 hour urinalysis showed no issues with anything other than high urine pH (6.772), a SSCaP of 102 and high citrate (214). I eat a mostly vegetarian diet keeping sodium and added sugars within reasonable limits with only occasional small portions of chicken or seafood. Any suggestions for bringing the pH and citrate levels to a healthier range? I can only physically drink about 50 oz. of fluid a day maximum so that is not an alterable factor.
Also, to insure I consume enough calcium, would small doses of calcium citrate be safe to take on occasion?
Hi Lydia, High pH and low citrate typify calcium phosphate stone formers. I am guessing your urine calcium is above 200 mg/d (‘normal’ but raises risk for stones). Oxalate may well be a minor issue for you, if one at all. As I have no other details, that is all I can say, and your physicians will need to take proper steps. As for calcium citrate, it is an approved calcium supplement. Foods with calcium are always prefered if possible. Regards, Fred Coe
I eat a mostly vegetarian diet (only small portions of poultry or seafood once or twice a week at most) yet my urine pH is 6.772. Every year it goes up despite my healthy diet. What am I doing wrong? And what can I do to fix this?
Hi Lydia,
Are you on any supplements that are increasing your pH (like potassium citrate or mag citrate)? Also, eating a veggie diet is wonderful but can increase urine pH. We don’t really care about a high urine pH in stone disease UNLESS you also have high urine calcium, and low urine volume. Do you?
LMK-
Jill
Will having a glass of fresh lemon water each morning help disolve kidney stones and prevent more from occurring?
Hi Mick, in a word, no. Here is a pretty good summary about how you might approach stone prevention. Regards, Fred Coe
I like this article. I got the “list” from my doctor, and when I looked up things I could and couldn’t have, they differed greatly. When I asked him, he said he just liked it. Your information is backed up . Thankyou.
Is there any information you can give on oat milk .
Thank you
Charles
Hi Charles,
We do have some research on it. Go here: kidneystonediet.com/resource-list for specifics on sub milks and oxalate.
Nurse Jill
Hi there,
I have read that soy is high in oxalates, but is this for all types of soy products?
I notice that soy monoglycerides and soy lecithin are in lots of items, are they as high in oxalate as soy protein?
Is there really any way to know?
Jim
The dose makes the poison. You can still eat soy and soy products. Read this:https://kidneystonediet.com/why-do-oxalate-levels-vary/
Warmly, Nurse Jill
Why are grits so high in oxalate, while corn and corn flour are not?
Hi Joy,
I would assume bc the germ is still intact in the grits while it is removed in the flour. And the germ will have much more oxalate. That being said, you can still eat grits, just have with a calcium containing product and don’t over consume. Once a week is just fine to fit into a lower oxalate diet. Also read why oxalate levels vary from list to list here;https://kidneystonediet.com/why-do-oxalate-levels-vary/
Warmly, Nurse Jill
Since 2018 I have had no less than 4 procedures a year (2 per kidney) to remove stones either by laser litho or EWSL. It’s been a nightmare challenge. I had weight loss surgery in 2015 and the stone production was incredibly exacerbated by this malabsorptive procedure (Duodenal Switch). I have been on 15 meq of Potassium Citrate 4X daily for years and I take Calcium Citrate as well as part of my bariatric vitamin regimen. In late 2022 I started desperately researching dietary info for Calcium Oxalate stones and found someone named Sally K Norton who had a ton of info including PDF documents that listed food levels and their oxalate mg and wither it was very low, low, medium, high or very high. I started following this religiously cutting out all foods that were high. In January, 2023 I knew I had a kidney stone because I was scheduled for another laser removal of stones from my right kidney. I went to the bathroom and proceeded to pass 24 stones in varying sizes at one shot. I have the photos. I’ll spare you (LOL). I still went in for the procedure and when I came out in recovery my Urologist told me that kidney was all clear. A few weeks later a CT scan of both kidneys ureters and my bladder showed no stones. I have not had a kidney stone since then (it’s been 15 months). I love this website (my nephrologist at University of Louisville told me about it) and am double checking all my info to make sure I am still on track. I hope to never have another kidney stone and will continue to pass this info on to my friends who ask me about my stones and what I did to treat them.
Hi Tony, malabsorptive procedures raise urine oxalate and lower urine volume and citrate. You should be followed using 24 hour urine collections to monitor stone risk, and also risk for kidney injury. Duodenal switch is a major procedure. Best, Fred Coe
I’m a POTS patient who also had a 21mm calcium stone. 3-4,000mg/ sodium per day is what I need to feel somewhat normal (drinking it in the form of LMNT). Any ideas on how to offset the sodium or am I doomed to for another? I was diagnosed with POTS after the kidney stone and was not eating much sodium because I hate salt.
Hi Ashley, postural hypotension was diagnosed after a kidney stone, so I gather you ate a low sodium diet before that without symptoms. Since you hate salt, you must have had a low sodium diet for years. So I am unclear about what is wrong. As for the stone, it would have formed before the diagnosis of POTS. Certainly you would want a full evaluation, and see what causes of stones might be amenable to treatment. If possible do the 24 hour urines on a diet like that preceding your stone. Regards, Fred Coe
Since water is drained ar the end of cooking, how do you count the salt you put in the boiling water for pasta?
Hi Kay, I cannot count it. Some no doubt penetrated into the food water, some is lost. To fractionate these two sodium pools would require an analytical lab. Fred
Why is cooked spinach worse than raw on this list? Cooking decreases oxalate content. It’s extremely misleading, dangerously so I would say because it gives people the impression that raw foods are safer than cooked. It says it’s per serving size, but that’s such a horrid, eyeballing method of measuring anything that I cannot believe any serious agency would ever list it especially without actually writing what the serving size is! This is worthy of a high school homework, not a serious organisation people rely on for health information. You cannot list the amount and say it’s for a unit nobody can actually measure!
Hi John, I am afraid that, as stated in the article, the high school is the Harvard School of Public Health. They provided the sources for us. I believe people in general use serving size as being familiar. Because oxalic acid is leached out of the leaves and more available for absorption, cooked spinach can have more bioavailable oxalate than raw. Of course cooking time and drainage matter. The site has a lot more on oxalate. Diet oxalate is not always important. An ideal kidney stone prevention diet has defenses against diet oxalate. Regards, Fred Coe
Hello,
I see the article cautions against lemonade due to being high in oxalates. However, as I understand it, lemonade contains citrates which are supposed to hinder stone formation and lemonade is often recommended to stone formers. Can you clarify? Thanks.
Hi Chris, It is true that an article on oxalate narrows one’s aspect. Lemonade is complex. If the lemons are ripe citrate will rise in urine because the citric acid in the drink will be mainly anionic. If the lemons are less ripe and the drink more acid the citric acid will be just that and urine citrate will not rise. Thus the caveat. Regards, Fred
Is there any data supporting specific amounts of oxalates to be safely consumed per day such as an upper limit, to help with stone prevention?
Hi Laura, as a (very) general rule, 100 mg/d or less is good, and I think below 150 mg/d is fine if diet calcium is at least 800 mg/d and higher oxalate foods are taken with some calcium containing foods. Regards, Fred Coe
what is the oxalate level of Acai berries?
Hi Kathy, I made a Perplexity search for oxalate content of these berries and there appears to be no measurements in reputable sources. https://www.perplexity.ai/search/amouont-of-oxalate-in-3-grams-kRFtPL.XQaOH3fzZVKJPeg#5 One must presume there is some, as all berries have some, but no one has measured thus far. Best, Fred Coe
I have read that having a glass of milk with your meals helps with absorption of oxalates. My question is how much should you have? I am not a big milk drinker but would like to try and add to my meals but how much is “a glass”? Thank you.
Hi Ann, Because calcium links to oxalate in the GI tract, any dairy product will reduce oxalate absorption. So a good principle for calcium oxalate stone formers is to add some kind of dairy along with veggies or salads, or fruits known to contain considerable amounts of oxalate. Best, Fred Coe
I have had 5 surgeries/procedures to remove kidney stones…..I was told low oxalate diet. I am so confused by all the information that I was given I can’t even absorb it. My question is for calcium oxalate stones…More calcium or less calcium, calcium with every meal and is chicken and fish high in oxalate? I like Speical K cereal is this bad to have for breakfast with an english muffin? I saw a nutritionist and I am more confused as ever.
Hi Roxane, Here is my best introduction about what to do. See if it helps. Fred
I have been suffering from kidney stones for almost 25 years now and it’s re-occurring every 6 months, it has always passed on its own. But in Aug I had to get a surgery for 7mm stuck in the ureter, was infected with enterococcus has sepsis and several septic attacks. Glad to be here to read through this list. I also have OAS, and the stones are calcium oxalate. Thanks for the nice article and an extensive list.
Hi Vasanth, I strongly advise you get evaluated and treated based on cause of the stones.Oxalate is rarely the main issue by itself. Do not rely on low oxalate diet. Regards, Fred Coe
Hello- thanks so much for all of this helpful information! I’m trying to make sense of when corn products are a concern- fresh corn, popped corn, corn flour all seem to be ok, but grits are higher in oxalate as is cornmeal. Why would the whole dried corn (popcorn) be ok, but grits aren’t? Thanks for any clarification you can provide.
Hi, Sorry to be so late. It is all in the amounts of food product. Grits are processed so as to release oxalate and a serving of grits provides more actual food mass – less air – than poped corn. Best, Fred Coe
Hello, I recently turned 70 and have now had two laser surgeries for stones in my ureters (a 5mm stone in 2019 and a 1 cm stone two weeks ago). Sadly, my urologist from 5 years ago never gave me a urine test, but my current urologist is having me do one in a few weeks. The first stone was oxalate and my current urologist told me my most recent one was as well (waiting for the post-surgery lab results for confirmation)., Five years ago urologist #1 put me on 6 month check ups and just told me to drink a lot and avoid spinach, chocolate and tea (which I did)– but no urine test. I did as he said, but what I didn’t do was was watch my sodium or watch the OTHER oxalates in my vegetarian diet which, once we started doing the math last month were through the ceiling. I wasn’t eating spinach the last five years, but I was eating was A LOT of almonds, cashews, walnuts, tofu, grits, miso, pinto beans, black beans and an enormous amount of whole wheat flour breads and bagels, pasta, figs and dates. I’d estimate my sodium intake over that five year period after stone #1 was double or triple the 1500mg recommended. After they discovered stone #2 (and a lot of calcifications) last October in a CT scan, we finally discovered you guys. I have two questions before my urine test. We’ve already tweaked the diet to your recommendations (daily oxalates below 100mg and calcium around 800mg). So I intend to do what Jill recommends before the urine test: go back to my old diet. Do I do that for just one day prior to the test? My second question is for a follow up urine test. My urologist told me his follow up is one year after the first. Is there any way to get one sooner? I’m not sure if he’s amenable to that, or if my insurance will cover it a month later. Thanks for all you do at this site!
Hi JT, zi would test as you are, and see what your risk is. When you make a change, if needed, insurance generally pays for followup as needed. I changed your name to initials as requested. Best, Fred Coe
When you say “test as you are, and see what your risk is” do you mean go back to the diet that resulted in my two kidney stones the day before the test? Or, would you advise taking the urine test with the low oxalate and lower sodium diet that I’ve been on for the last month? Thanks…
Hi JT, with the new diet to see if it worked. Fred
Do you do personal phone consults?
Hi Susan, I do telehealth. 773 702 6134 will get you to the people who can help with this. Regards, Fred Coe
I have a kidney stone blockage and stent at the moment. I also had a UTI (went away with antibiotics after my stent surgery) and now another UTI 2 weeks later. I find that cranberries (Azo or CranRx) helps my UTI pain, but I also see that berries are oxalates and not good for kidney stones. So I’m unsure what to do. Its been 3 days on the antibiotic w/o reduction in pain and the only way I can get through my work day is with cranberries. But I don’t want to add to my kidney stone either. Anything else I can do to help my UTI pain (since its not subsiding with antibiotic use)? Or can I go ahead with the cranberries temporarily?
Hi Susan, The stone itself is a surgical issue that will resolve. Prevention requires proper testing for causes. I would advise that so you can plan long term prevention. Stones removed must be analysed. Regards, Fred Coe
Hi,
Thank you for such an informative post. I’ve been passing calcium oxalate since I was 16 (now 32). I have high urine calcium. My docotors throughout the years always want me doing a low oxalate diet, but then they never provide me with any further information. I get overwhelmed, and give up.
My main concern is: I have dairy, gluten, and soy intolerances and have to avoid them too. Not a big deal with gluten and soy it seems, when both seem to be high in oxalate. But the issue I’m dealing with is getting enough calcium being dairy free. Do you have any advice here?
Hi Natasha, Your high urine calcium is more likely the cause of ongoing stones assuming your diet has controlled the oxalate. It is a target for stone prevention. Low diet calcium is the worst possible treatment for it as you have a skeleton and that kind of diet raises urine oxalate. Best, Fred Coe
I am a vegetarian and eat mostly oxalate rich foods. I have severe osteoporosis and don’t want it to become worse. I have never had stones, nor have I been tested for oxalates. What can I do take as far as supplements to combat these oxalates? I will limit my nut intake.
Thank you for your help
Hi Ellen, I wonder if your diet is deficient in calcium – bone disease. You are not a stone former, and therefore urine oxalate may not be high or may not matter because of other urine factors – like low urine calcium. I would suggest 24 hour urine testing would clarify both urine oxalate and calcium, as off hand I worry the latter may be present and not ideal for bones. Regards, Fred Coe
Thank you, very much, for this website and the information contained. It definitely helps to paint a clearer picture of what, what not, and how much to eat. I have been recently diagnosed with stage 3a CKD and oxalate stones. I have only (knowingly) passed one stone to date (2021). Several more remain firmly nestled in both kidneys. I am working with a nephrologist, and currently on (attempting) a low oxalate diet and supplementing with 1300mg sodium bicarbonate, daily. The problem(s) I am encountering is getting clear and consistent data on the oxalate content of various herbs, spices, chile peppers, and different varieties of foods in the same family (i.e. sweet cherries vs. tart cherries). I’ve also noticed that hummus is sometimes considered OK, even on this site. I that with the caveat it does not contain tahini (which isn’t usually the case)? Is there another database you recommend using?
Hi James, Is your urine oxalate high? If so, is your diet calcium high enough to prevent excessive oxalate absorption? Usually diet oxalate is not the problem and eliminating all oxalate an ineffective measure. A better diet alternative is high calcium reduced sodium moderate oxalate. Best, Fred Coe
What about the packets of hot chocolate mix, like Swiss Miss? Are they lower oxalate than homemade hot chocolate?
Hi Jenny, I am afraid not. It is all the same. But if you have milk with the chocolate oxalate will not be absorbed well. Is your urine oxalate high? Are you sure low diet oxalate is important for you?? Best, Fred Coe
ello- thanks so much for all of this helpful information! I’m trying to make sense of when corn products are a concern- fresh corn, popped corn, corn flour all seem to be ok, but grits are higher in oxalate as is cornmeal.
Could my hand and leg pain at night be from high oxalate food? i noticed that my hands were on fire at night when I drank kale/beet smoothies, then stopped when I stopped drinking them. This happened a few times.
Hi ELizabeth, No. Food oxalate has no role in causing leg pain. Possibly smoothies of kale and beet changed blood bicarbonate or calcium or glucose, but oxalate is not the culprit. Best, Fred Coe
Can a diet high in oxylates contribute to macular degeneration?
Hi Melanie, I know of no information linking diet oxalate to macular degeneration. I doubt it is plausible given blood oxalate levels are quite low. REgards, Fred Coe