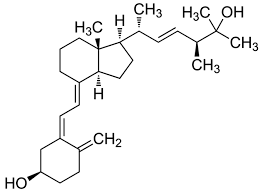
 Not rarely patients and readers on this site ask about vitamin D supplements and whether they raise the risk for kidney stones or reduce risk for bone fractures. This article is about the first question. In pursuit of the answer, I would like to share with you how one can come to know the ‘answer’. It is not magic. Given modern access to PubMed many patients could come to a reasonable answer without me. The large image is of 25 hydroxy vitamin D (25D3). Liver cells make it from the vitamin D3 we buy OTC by adding the OH (hydroxyl) group at the 25 position (between the two ‘CH3s’ at the upper right. It is active on bone and GI tract calcium absorption. 25D3 is what we measure as ‘serum vitamin D level’. Kidneys add an additional OH (hydroxyl) group at the 1 position (lower left at ‘noon’ above the OH facing left on the figure). This is the most active form of vitamin D.
Not rarely patients and readers on this site ask about vitamin D supplements and whether they raise the risk for kidney stones or reduce risk for bone fractures. This article is about the first question. In pursuit of the answer, I would like to share with you how one can come to know the ‘answer’. It is not magic. Given modern access to PubMed many patients could come to a reasonable answer without me. The large image is of 25 hydroxy vitamin D (25D3). Liver cells make it from the vitamin D3 we buy OTC by adding the OH (hydroxyl) group at the 25 position (between the two ‘CH3s’ at the upper right. It is active on bone and GI tract calcium absorption. 25D3 is what we measure as ‘serum vitamin D level’. Kidneys add an additional OH (hydroxyl) group at the 1 position (lower left at ‘noon’ above the OH facing left on the figure). This is the most active form of vitamin D.
Find Papers With Answers
Use PubMed
PubMed is a US government site open to the world. It has lookup just like Google (perhaps not as well done, but I am not an expert in such matters). I opened the site and said: “Vitamin D and kidney stones”, and limited my search to humans and trials or prospective randomized trials. This way I got a mix of the two kinds of human trials on this subject. Some other papers showed up, not quite what I wanted. You could tell if you went in and looked.
Read the Papers
I found 12 trials that seemed reasonably useful, and I read them. Sometimes publishers will not let you read the whole thing but just the abstract. That alone is usually enough to get the final opinion of the authors. At universities we get more access because libraries pay for subscriptions. Recently I reviewed a science paper and illustrated how to use the objective as a reading guide. I will do the same here, but it is easier. Trials 7are very direct. Authors are clear about the goal and put it up front. The logic between what they desire and what they do is usually very simple, even if the methods and techniques are themselves elaborate. To the 12 I added one meta-analysis. In these, statisticians pool data from many trials using methods that field has agreed upon, in general. The purpose is a general sense of what trials in the aggregate have to say.
A Spoiler
For those with better to do than wade through the trial data concerning vitamin D and calcium supplements: Vitamin D does not of itself appear to increase risk of kidney stones. Calcium supplements given with vitamin D supplements appear to raise urine calcium and stone risk, and in at least one very well done trial raise the rate of actual new stone formation. The message: Vitamin D + calcium supplements may well increase kidney stones, but vitamin D alone does not seem to do this.
Randomized Controlled Trials
One Trial Is Good As An Example of the Science
To begin, no trials of this class have addressed kidney stones per se. All are in quest of other primary information. But along the way they included whether or not new stones formed, or in some cases, whether urine chemistries varied in a decisive way toward increased kidney stone risk. 2021: An RCT asked if vitamin D reduced risk of falling. Let’s take a look at their objective – what they were after: “We sought to determine whether monthly high-dose vitamin D supplementation reduces risk and incidence of falls.” But they did not themselves collect any new data. Instead they took the data from a trial they had performed in Australia whose objective concerned vitamin D effects in elderly people on mortality, total cancer and specifically colon and rectal cancer. Falls was one of the ‘pre-specified tertiary outcomes’. This last mouthful means mortality was first, cancers were second, and falls third. ‘Pre-specified’ is a big deal in trials. It means they set out to look at the effects of vitamin D supplements. The alternative is to look around at the end and see what D might or might not have done for other aspects of health and disease. That alternative is much weaker. First of all, chance can play a role. You collect a lot of information in trials, and by chance the treated patients may have had, for example, fewer or more kidney stones. But pre-specified means you cannot just look around, you have put your flag down at the beginning. Let’s pause a moment and look at how a trial is set up. They said it well: “Between February 2014 and May 2015, 21, 315 participants aged 60-84 years were randomized (1:1) to monthly doses of either 60, 000 IU of cholecalciferol or placebo for a maximum of 5 years. People who reported a history of osteomalacia, sarcoidosis, hyperparathyroidism, hypercalcaemia or kidney stones or who were taking >500 IU/day supplementary vitamin D were ineligible. Falls, a pre-specified tertiary outcome, were ascertained using annual surveys and, for a subset of participants, 3-month falls diaries. The primary outcome for this analysis was any fall in the month before completing an annual survey.” So within a pool of participants some are randomized (allocated using random numbers) to either 60,000 u/month of vitamin D or to a lookalike placebo (controls), and observed for some years thereafter (prospective): A randomized controlled prospective trial (RCT). In brief, they found no effects of high dose vitamin D on falls. Along the way, they note: “The incidence of hypercalcaemia and kidney stones did not differ between groups.” Incidence means new onset rate. They know this because it is prospective – they gave the two groups high Vitamin D dosing or placebo and observed them over five years, so they could time the occurrence of something new. So what do we have from this trial? Only that 2000 U daily (60,000/month) did not raise the incidence rate of kidney stones. But that is not firm. Kidney stones were not a pre-specified outcome. This means that the study was not ‘powered’ to determine stone risk. Given the assumed rate of new stones among normal people the subjects in the trial may not be large enough to produce enough new stones to detect a difference between the vitamin D and control groups. Likewise, stone onset was not pursued with the vigor of death, cancer, or falls, so perhaps not all were detected.
The Other RCT Function Similarly
2019 RCT of Vitamin D or Omega – fatty acids On Progression of Kidney Disease in Diabetic Patients. This was a 2×2 design: 1312 patients with diabetes were randomized to the two treatments or placebo thusly – Vitamin D, the fatty acid, both, neither for five years, with a primary endpoint of change in kidney function. It was a very well done trial. Briefly, the two treatments had no effect on kidney function (unsuccessful treatments). From the total over five years, 58 patients formed kidney stones, 32 received vitamin D 26 did not (no significant difference). But as in the prior trial kidney stones were not a pre-specified outcome so the study was not powered to detect an effect of Vitamin D. 2018: RCT of High Monthly Vitamin D on CV disease, Respiratory infections, and Falls: No increase in stones. 5110 people in Auckland, New Zealand, were randomized to 100,000 U/month (3,333 U/d) of vitamin D or look alike placebo and followed for an average of 3.3 years. Although not a primary study endpoint, subjects were sent a monthly (years 1 – 2) and every 4 months (year 2 – 3) questionnaire which included: “Since you took your last capsule (about one month ago) have you been diagnosed by a doctor as suffering from any of the following conditions?…” one of which was “Kidney stones”, with “Yes/No” response options.” Serum 25D levels were measured in a sample of drug and placebo subjects. Both averaged 60 mol/l at the start, with the supplement group rising to about 120 vs, no change in placebo controls. Among vitamin D treated people 76/2439 reported a new stone (3%) vs. 82/517 (3.3%) of placebo cases, p, NS. The hazard ratio was 0.62, with a 95% CI of 0.24, 1.26. Of interest, mean serum calcium values did not differ throughout the trial. Since stones were not a pre-specified outcome, the lack of a significant effect need not mean vitamin D had no effect. 2018 RCT of High Dose VIt D on Serum and Urine Calcium. A total of 132 women were randomized to 10,000 U/d of vitamin D + 1,200 mg calcium carbonate vs. 600 U/d of vitamin D + 1,200 mg calcium carbonate and followed for 6 visits: 2 baseline and 4, at 3 month intervals during the treatment phase at which serum and urine calcium and serum PTH (and other things) wer measured. Although small, the study is not inadequate for the purposes as endpoints are easily measure chemical values. Urine calcium at baseline was the same for both groups (121 vs 117, high dose/low dose D). During treatment it rose in the high D to 229 vs. 168. These differences were not statistically significant. The authors report 34 of the high D subjects had 72 24 hour urine measurements above 250 mg/d vs. 19 subjects (35 24 hour urine in the low D group (p<0.01 for the difference using a proper statistic). The most reasonable interpretation is that high vitamin D with high calcium intake can indeed raise urine calcium more than one would find without extra vitamin D. The authors comment that the increased stone rate in the 2006 RCT (below) could have reflected their use of high calcium intake. Visitors to this site should not be surprised by the effect of calcium supplements on urine calcium, as nothing was done to control sodium intake in either study. We never would propose high calcium intakes without sodium control. 2017: An RCT on effects of Vitamin D and 1500 mg/day of calcium on cancer. Because we have already explored how randomized controlled trials work, I shan’t repeat the details. This one was performed in Nebraska using post-menopausal women, and concerned treatment with Vitamin D 2000 U/d + calcium carbonate 500 mg tables 3 times a day or look alike placebo tablets for both. The primary outcome was any kind of cancer. Secondary outcomes were kinds of cancers and a list: hypertension, cardiovascular disease, osteoarthritis, colon adenomas (benign), diabetes, upper respiratory infections and falls. All were incidence rates, this being a prospective trial. Where are kidney stones? In the discussion, the authors note that the rates of stone incidence did not differ between treated and control groups nor did the incidence rate in the treated group differ from incidence rates in prospective population studies (Ask people about stones every year or so as they age). So, no increase in stones. Of course, the study was not powered to detect a difference in kidney stone incidence. 2016 RCT of High Monthly Vitamin D on Upper Respiratory Infections: No increase in stones. A small trial in which 55 older adults were given vitamin D 100,000 U/month (3,333 U/d) vs. 52 who received standard dosing (400 – 1000 U/d or 12,000 U/month) for one year. This may seem a paltry study, and is, except it focused on elderly people in long term care institutions. For stones, none in either group. For infections the high D intake led to a fall (HR = 0.66 (0.38-0.94 95% CI). Falls were more frequent (HR = 2.3 (1.49-3.63 CI). I included this to point out that small studies, even RCT, can give odd outcomes because a few more or less infections or falls have excessive power over the outcome. I mean no criticism of the work which was well done, nor am I against small trials for insight. But if one proposes high dose D against respiratory infections as a wide spread medical initiative one must do a larger study. As for stones, the lack of effect means little as the study is very under powered. 2014 RCT of Vitamin D repletion + Calcium in Postmenopausal women on Serum and Urine Calcium. A total of 163 women was assigned to vitamin D repletion of “400, 800, 1,600, 2,400, 3,200, 4,000, or 4,800 IU/day, or placebo.” Calcium citrate was added based on diet calcium intake assent to achieve 1,200 mg/d. The trial lasted one year, and serum and urine samples were collected at 1, 6, 9 and 12 months. They found that urine calcium rose with vitamin D repletion but increasing vitamin D dose did not raise urine calcium. The frequency of very high urine calcium excretion (>300 mg/d) also was not related to vitamin D dose. They found that baseline (before repletion) urine calcium and age were the only predictors of high urine calcium with treatment, age lowering the risk baseline urine calcium correlating positively with risk. This latter is no surprise to those of us who read (or write) this site, as baseline values help identify women with genetic hypercalciuria. Of greatest importance, urine calcium in the vitamin D placebo was no different from those receiving vitamin D. High diet calcium, not vitamin D appeared to raise urine calcium and stone risk. 2006: An RCT of calcium and Vitamin D on bone fractures showed increased stone risk in postmenopausal women. Among the 68,132 women in the Women’s Health Initiative 36,282 were randomly assigned to either two daily tablets each containing 500 mg of calcium as calcium carbonate + 200 U of Vitamin D or lookalike placebo tablets. Women with prior kidney stones were excluded. The primary endpoints were fractures, spine, hip, and elsewhere, and the working hypothesis was that the combination of extra calcium and vitamin D would reduce fractures. Of interest here, stone risk increased (hazard ratio 1.17 (1.02 to 1.34), mean and 95% confidence limits. Fracture rates were not reduced. This study helped found the search for a vitamin D – kidney stone link. Looking back on it, from our knowledge of all of the other trials, calcium intake was greatly increased and could have caused stones. Also, the study was very large and therefore had the power to detect a difference in stone incident rates.
A Meta-analysis of Available Trials
2016 Meta-analysis of Vitamin D Effects on Urine Calcium and Kidney Stones. This kind of analysis pools data from large numbers of publications, as much as possible RCT but sometimes also observational studies. The authors use established and generally agreed upon methods to judge the quality of the studies they include and also the kinds of statistics that are most appropriate. So, although most of us are not privy to the details we can assure ourselves that those who publish these influential overviews can be relied on to adhere to formulaic approaches. That said, what about this paper? From the world’s publications they found 48 studies (45 RCT, 3 open label) appropriate for inclusion concerning high serum and urine calcium and kidney stones from vitamin D supplementation with or without added calcium. These 48 studies included 10,279 subjects who did and 9554 who did not receive vitamin D supplements (total = 19,833). From this ensemble 17,801 people had reported serum calcium levels and among them vitamin D supplement was associated with increased risk of hypercalcemia (p=0.01). Their analysis also noted that calcium supplementation increased risk of hypercalcemia even more than vitamin D. For hypercalciuria they had only 1,987 subjects from all of the studies. They defined hypercalciuria using the older criteria of >250 mg/d (women) and >300 mg/d (men) or a urine calcium to creatinine ratio of >3 mg/mg. We now realize these criteria are far too high, as stone risk is detectable urine calcium excretions >200 mg/d in either sex. Even so, vitamin D supplements increased risk for hypercalciuria as they defined it (HR = 1.94, 1.06-2.53 95% CI). However with analysis of correlations urine calcium appeared to increase with calcium supplements but not with the amount of vitamin D, so calcium intake seems the main driver of urine calcium. For stones they had data for 9619 subjects and there was no increased risk. Although not itself an RCT for stones, the study had enough subjects that it could reliably detect an effect of vitamin D on stone incidence.
A Few Smaller Studies I Do Not Wish to Detail
I said I had 12 trials plus a meta-analysis and here are the other four I did not review for you. Small observational report showing no risk for hypercalciuria and stones with vitamin D Brief trial showing vitamin D repletion did not increase risk of kidney stones Brief trial showing that repletion of vitamin D deficiency does not raise urine calcium or risk of new stones Small trial showing that vitamin D does not increase urine risk factors for kidney stones in postmenopausal women with osteoporosis You might wonder that I do not open each of these trials and show more, but since they more or less accord with the larger trials and are small enough and short enough that effects on stone formation would lack sensitivity I have not chosen that course. The links will open to their summaries for those with an appetite for more.
This Has Been a Tedious Article to Write
If I may step before the curtains for a moment and tell you how I feel, it is this. Trials are the main stay of clinical medicine but – how can I say this? – boring. Each seems to me a long sermon, filled with wisdom and best when short. All trials share the same chassis, the same design. They need to. All trial reports, thusly, read about the same. Few authors just plain out say what they found. It is all – properly – coated with sage reservations, and hemmed in with proper concerns for the ultimate truth. In fact, almost all I read end up calling for – you guessed it – another trial!. This is not criticism, just sideline carping by someone who reveres trialists for their amazing patience and willingness to wade oceans of detail but sighs at the beginning of every trial report. It would appear that respect leads to love no more than vitamin D supplements to kidney stones.
What Can I Say to Patients, to Physicians
Nothing supports the claim that vitamin D supplements themselves cause stones. Many studies support the claim that when you combine vitamin D supplements with ample calcium supplements – in the range of 1,000 mg/d or more – urine stone risk factors rise, and in the one large trial from Women’s Health Initiative – stone rates increased. This site already says more or less the same. We consider calcium supplements part of the kidney stone diet but only when diet sodium is controlled to below 100 mEq/d and when 24 hour urine testing offers some safety. I suppose you might say had I or another expert on stones been part of the design team nobody would be offered hefty calcium supplements and vitamin D supplements without both of these precautions. So if in a stone former vitamin D levels are low and require supplements I would give them, but I would measure 24 hour urine response. I would not at the same time give calcium supplements unless diet sodium were being controlled and 24 hour urine measurements had confirmed this was indeed the case. But – the word that ends all scientific conversations, none of the negative studies were powered to detect a difference in new stone incidence from vitamin D supplements except the one what showed a difference. Only the meta-analysis can stand against that large and famous women’s study. This underlines what I just said. For stone formers. use the supplements when needed but with precaution.

Dr. Coe,
Thank you for your ongoing contributions to this site and stone disease in general…it’s much appreciated!
Can you please clarify your bolded statement at the top of the article? If I’m understanding the various forms of the D sterols, the form we buy OTC is not calcidiol (ie 25vitD), but rather is the inert form (similar to the natively generated form from UV light), correct?
Thanks again.
Hi Stephen, Thanks. It is indeed and I will correct the statement. Much obliged! Fred
Dear Dr. Coe:
Is there any correlation between taking dietary Magnesium and increased urine calcium? I take 590 mg of Magnesium Beta Hydroxybutyrate per day as a neuro protectant and have noticed that my urine calcium is now 351mg/day. Perhaps this is just a coincidence?
Hi Lisa, The butyrate can impose a significant acid load that raises urine calcium. Regards, Fred Coe
Dear Dr. Coe, I have been diagnosed with hyperoxaluria, and previously diagnosed with hypercalciuria (now on a thiazide and low sodium diet). I have been advised to increase diet calcium and take a calcium supplement. The diet part is difficult for me for various reasons. I am taking a calcium citrate supplement with meals, particularly high oxalate meals. I understand that calcium binds oxalate in my gut therefore preventing absorption. I have also read that magnesium can also accomplish this. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3883082/
What do you think about lowering my calcium supplement by about a third and replacing that with some form of magnesium at the same time?
Can you advise how many mg of calcium supplement I should be taking with each meal?
Hi Thomas, This is a complex issue and I cannot comment in detail as I do not know your entire medical situation. The kidney stone diet uses low diet sodium to lower urine calcium and ample food calcium to lower urine oxalate. One seeks a diet (24 hour urine) sodium of 1500 mg. THiazide is added when urine calcium is still too high. Reduced diet oxalate is also used to lower diet oxalate. No trial data support magnesium for stone prevention. Regards, Fred Coe
Do you have any insight into whether potentially excessive vitamin D supplementation in 3rd trimester of pregnancy (5000u-10000u a day) might potentially lead to increased stone formation in offspring.
Hi Mara, I doubt it will affect the offspring but have no information about the subject. That is a very large dose of vitamin D, however. Regards, Fred Coe
Hi, Dr. Coe:
I am a stone former. I had surgery a few years ago to remove some calcium oxalate stones. My doctor put me on Calcium Citrate supplements. I try to follow a low oxalate kidney stone diet. (Although that is hard to do because there is a lot of conflicting information, and there seems to be no authoritative source of information about how much oxalate there is in various foods.) I have restricted sodium in my diet for many years, even before my kidney stone episode, simply because I believe a low-sodium diet is healthy for a number of reasons. I felt that I was doing well by following my doctors’ orders. But recently, I had some alarming symptoms that I feared might be kidney stones. And two days ago, I passed a 5.6 ml x 4.4 ml x 2.4 ml stone. I thought I had been doing everything right, but I hadn’t been. I had slacked off a little bit on my water consumption, although I was still trying to drink more than normal. I started taking a collagen supplement–12 grams a day. And I got the bright idea that Vitamin D was a very beneficial vitamin and that I should take the maximum safe dose–4,000 IU a day. Only, after I had the new kidney stone episode did it occur to me that since collagen supplements are animal protein, I probably should have been cautious about adding them to my diet. And only after reading this article did I discover that a large dose of Vitamin D might not be such a good idea. And I did these things without informing my doctors. If my doctors had known about what I was doing, they probably would have stopped me. I am just writing this as a word of caution to my fellow stone formers: Talk to your doctor before you make any changes in your habits or supplements or diet.
Hi Dennis, I think you should get a full evaluation for causes of stones even though your thoughts about the collagen and high vitamin D are indeed on target. Regards, Fred Coe
Can kidney stones cause overall inflammation in the body? Last fall in two separate incidents I developed tendonitis, one in ankle, one in shoulder. 18 mnths ago I was told I had some small stones that should pass on their own. This morning I had two of those stones removed by laser. It seemed as though my tendinitis was getting progressively worse and I am hoping getting these stones out might quiet the ovrall inflammation? Thanks.
Sandi
Hi Sandi, stones do cause inflammation within kidneys, and stone surgery and stone passage cause transient inflammation whose inflammatory mediators are in the blood and can worsen symptoms at sites of prior injury. As the urinary system comes back to normal one might hope the same at the joints. Regards, Fred Coe
Dear Dr. Coe,
I’m trying to figure out whether it’s safe for me, given my overall health picture, to take 4000 IU of Vitamin D as my endocrinologist is suggesting or whether it would put me at serious kidney stone risk. I am a 56 year old and was diagnosed with a “hot” thyroid nodule 16 years ago, for which I was treated with radioactive iodine (and am now on Synthroid). Within weeks, I also had my first incident with a (calcium) kidney stone, which I was able to pass on my own. Eleven years later, I had a large calcium stone removed via ureteroscopy, at which time the imaging also revealed another, non-obstructing one, approximately 6 mm, in the other kidney (where it has remained and has so far not caused problems).
In the past year, a DEXA scan revealed that I have osteoporosis of the lumbar spine and osteopenia of both femoral necks. I have been working with an endocrinologist to form a treatment plan. My blood levels for most things were in normal range, including 10.0 MG/DL calcium. However, my creatinine and vitamin D levels were at the bottom of the normal range, 0.61 MG/DL and 30 NG/ML, respectively. Most concerning was that my Intact PTH was 90 PG/ML. My 24 hour urine tests showed mostly normal results, including 198 MG/24H for calcium. The abnormal result from the 24 hour urine was creatinine, which was 0.7 GM/24H. (Right now I’m not especially concerned about my creatinine levels, both because I had been eating a vegetarian diet in the 5 days preceding the blood/urine tests and because my eGFR was 105.)
My endocrinologist suspects that I have idiopathic hypercalciuria that is currently masked by my elevated PTH levels, which she wants to try to bring down by having me take 4000 IU of Vitamin D3 daily for several months before re-testing blood and 24 hour urine. I get adequate calcium from my diet and don’t take calcium supplements. I try to be careful of sodium intake. I also drink about 2.5 liters of water/day in addition to 24 oz. skim milk, 8 oz. of calcium and vitamin D fortified orange juice, and about 12 oz. of half-caffeinated coffee with milk. Do you think that taking that high a dose of Vitamin D supplements is likely to increase the size of my current kidney stone? My daughter is getting married in less than two months and I would like to avoid a kidney stone incident between now and then.
Thank you so much for this website and for your willingness to answer questions!
Hi Elizabeth, You are in a common quandary and need a way out. Do you have secondary or primary hyperparathyroidism? Let’s start with your creatinine. It measures muscle mass so low means low muscle mass – small person, perhaps not fit? It is not germane to anything. For your muscle mass (bone and muscle mass are in parallel) your urine calcium is high. Your serum PTH is high. Your one serum calcium is 10 which is possibly high. I would suggest that your physician stop any medications what might raise your serum calcium. Thereafter I would suggest several morning, fasting blood samples for calcium and PTH. The only real difference between primary and secondary hyperparathyroidism is the serum calcium. Depending on the results your treatment can be pursued in confidence. If secondary, vitamin D should be not unreasonable but your PTH might not fall. OFten glands are already large and over time serum calcium will rise requiring surgical cure. Regards, Fred Coe
Dear Dr. Coe,
I’m trying to figure out whether it’s safe for me, given my overall health picture, to take the 4000 IU of Vitamin D my endocrinologist suggests. I am a 56 year old woman and was diagnosed with a “hot” thyroid nodule 16 years ago, for which I was treated with radioactive iodine (and am now on Synthroid). Within weeks, I also had my first incident with a (calcium) kidney stone, which I was able to pass on my own. Eleven years later, I had a large calcium stone removed via ureteroscopy, at which time the imaging also revealed another non-obstructing one, approximately 6 mm in the other kidney (where it has remained and has so far not caused problems).
In the past year, a DEXA scan revealed that I have osteoporosis in the lumbar spine and osteopenia in both femoral necks. I have been working with an endocrinologist to form a treatment plan. My blood levels for most things were in normal range, including 10.0 MG/DL calcium. However, my creatinine and vitamin D levels were at the bottom of the normal range, 0.61 MG/DL and 30 NG/ML, respectively. Most concerning was that my Intact PTH was 90 PG/ML. My 24 hour urine tests showed mostly normal results, including 198 MG/24H for calcium. The only abnormal result from the 24 hour urine was creatinine, which was 0.7 GM/24H. (Right now I’m less concerned about my creatinine levels, both because I rarely eat red meat and had been eating a vegetarian diet in the 5 days preceding the blood/urine tests, and my eGFR was 105.)
My endocrinologist suspects that I have idiopathic hypercalciuria that is currently masked by my elevated PTH levels, which she wants to try to bring down by having me take 4000 IU of Vitamin D3 daily for several months before re-testing blood and 24 hour urine. I get adequate calcium from my diet and don’t take calcium supplements. I also drink about 2.5 liters of water/day in addition to 24 oz. skim milk, 8 oz. calcium and vitamin D fortified orange juice, and about 12 oz. of half-caffeinated coffee with milk. Do you think that taking 4000 IU of Vitamin D supplements is likely to increase the size of my current kidney stone? My daughter is getting married in less than two months and I would like to avoid a kidney stone emergency between now and then.
Thank you so much for this website and for your willingness to answer questions!