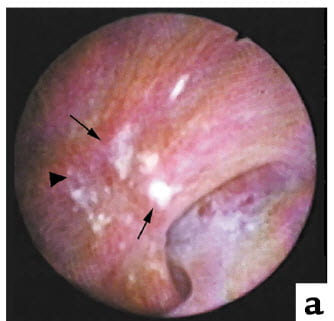
 The white clouds you can easily see on this human papillum are Randall’s plaque, named for the man who first described them. Stones grow on them. You can find bits of plaque and on such stones where they were once attached. Because plaque forms in and lies in the renal papillary tissue itself, bits of plaque on stones often carry with them fragments of tubules.
The white clouds you can easily see on this human papillum are Randall’s plaque, named for the man who first described them. Stones grow on them. You can find bits of plaque and on such stones where they were once attached. Because plaque forms in and lies in the renal papillary tissue itself, bits of plaque on stones often carry with them fragments of tubules.
This site has a long article detailing what we know about the facts of plaque, and rather than repeat it here is the link.
But how does this plaque come to be?
Who Would Care?
Scientists, of course. They measure things and imagine how they got the way they are. Then measure again to see if they have imagined rightly.
But physicians care, too, and patients. Once you know how something happens, know its ’cause’ as it were, you can fashion some treatment to prevent it, or at least slow it down.
So everybody has a stake in how something like plaque comes to be.
How Scientists Wrangle About ‘How’
They Fight Very Little About Measurements
Most of the time, measurements lead to few disputes. She says he measured wrong, he says she measured wrong. That rarely lasts long. Others measure, she and he and all the rest agree on the facts, and they all move on.
They Fight a Lot About Imagined Causes
You can see plaque. You can see stones grow on it. But you cannot ‘see’ the cause. It has been, so to speak. To ‘see’ it, you might put a camera inside a kidney, very time lapse indeed. But that might just show plaque growing.
It would be like seeing a glacier grow, or shrink.
Think About Global Warming
People have shown movies of glaciers shrinking. The cause is obvious enough – the Earth is heating up, so ice melts. No one doubts that ice melting means the temperature is going up.
But when we imagine the temperature is going up because we burn fossil fuels, and the released carbon dioxide traps heat in the atmosphere, fights start. How do you know we are doing it? The Earth has gone through many cycles of warmer and colder.
So you imagine we do it, and then perform the remarkable one thing we seem to have learned during the Renaissance: Make a deduction, and see if it is true.
People measure atmospheric carbon dioxide, for example.
Think About Plaque
What about plaque? It forms, for sure.
There are not that many ways to mineralize tissues.
One way is to create local supersaturations. That is how stones form, and tubules plug with crystals.
Another is to create special proteins that promote crystallization, like bone does – so called osteogenic calcification.
A third is when tissue dies – tiny patches of dead tissue will crystallize, presumably because living tissues resist crystal formation. Recent work on heart valve calcifications described both the osteogenic and dystrophic mechanisms.
These three components, mixed in variable proportions have given rise to three working hypotheses – dreams – that presently contend between each other for primacy. None of the three incorporate tissue death, whereas two require bone gene expression, and one local supersaturation. So of three imagined mechanisms, two are part of what people presently work on.
Scientific Deduction
The Form of It
If it happened this way, then we must find such is true. That is the formal shape of the deduction: If (x)…then (y). The testing of ‘y’ is to measure things, like in all science. The x is the imagined cause, a dream, a vision. It is a way around the opaque, hidden, ultimately unknowable workings of the world. The link – if…then, pure deduction.
From the imagined ‘how’, a string of logically correct links based on what we know for sure leads to some prediction we can verify by measuring things. That is how deduction works.
Stringency
Each link must meet the next one without any gap. Be sure you can make the measurements you need for verification.
Most important, the prediction must be necessary.
Necessary means that if the prediction prove false the dream is false. No means no.
Almost never will yes mean yes. Your prediction can be true over and over, test over test, but some other test prove it false. No is the end of the road, yes just a place along the way until someone, sometime, falsifies your dream.
Three Dreams About Plaque
As I mentioned in ‘Think About Plaque’, most wrangling right now is about three possible ’causes’ of plaque – working hypotheses, or dreams.
One is that papillary interstitial cells transform into osteoblasts, make bone matrix, and that matrix permits crystals to form. What makes them do this is not specified.
A second is vas washdown; calcium preloading of the vessels that nourish the deep papillum create tiny regions of supersaturations near thin limbs of Henle’s loop.
A third, proposed by Dr Marshall Stoller, is that calcifications much higher up in the medulla cause special conditions in the papillum that cause bone gene production by interstitial cells.
Bone Formation
In the late aughts professor Giovanni Gambaro described that cultured tissue from patients with medullary sponge kidneys expressed bone specific genes (link is to one of our papers summarizing his work). Given such tissues formed calcified regions, this led to the reasonable idea that bone gene expression could enable kidney cells to make plaque.
The idea led to a necessary prediction: One must find bone genes in regions of plaque in human kidneys. We found none. That should more or less make an end of the theory. But one might argue we did not measure enough genes to exclude all bone matrix proteins.
Vas Washdown
What is in the papillary tip
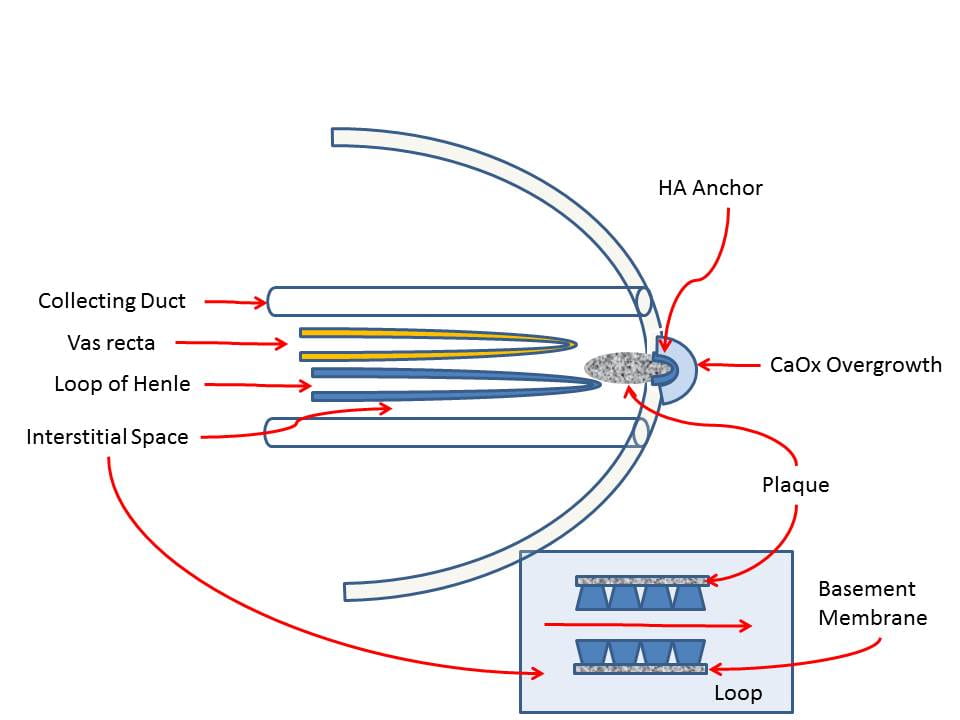 To the left is the tip of a renal papillum with a calcium oxalate stone growing over some plaque. The link above goes to an article with details of where things are.
To the left is the tip of a renal papillum with a calcium oxalate stone growing over some plaque. The link above goes to an article with details of where things are.
As always the plaque is calcium phosphate in the form of hydroxyapatite – the mineral of bone.
Plaque forms not inside of vessels (vas recta) or the tubules (collecting ducts and loops of Henle) that lie in the papillary tip, but between them, in the so called interstitium.
In your walls, the interstitium is the space between the pipes, between the air ducts, where mice or centipedes can crawl up from the basement to your bedroom and squeeze into it through a crack between the wall and an electrical outlet plate or bezel around an air duct, or the covering where a pipe comes into a radiator.
The vas recta
The descending vas recta bring blood down into the papillary tip. That blood flows into fine capillaries that branch off of the vessel and that I do not show in my drawing. Those same capillaries gather themselves together to form the ascending vas recta that brings the blood back up to the renal medulla (of which the papillum is an extension) and finally to the cortex and back to the heart through the renal veins.
The descending vas recta originate in bundles of larger vessels that course down from the cortex through the medulla on their way to the papillum. In the region of the medulla closest to the cortex, these bundles are surrounded by thick ascending limbs, each of which is an extension of a corresponding ascending thin limb.
These thick limbs transport calcium without water out of the tubule lumen into the surrounding interstitial space through which the vascular bundles must pass. The descending vessels convey the concentrated calcium down to the papillary tip creating supersaturation that in turn causes plaque.
The Loops
In the drawing I have shown plaque originating in the space surrounding the thin loops, because that is where we have found it.
The descending limb that brings fluid down from the cortex of the kidney is permeable to water because it contains aquaporin water channels. As it descends into the medulla and papillum water leaves because the interstitium of the medulla and papillum is higher in salts and urea than tubule fluid. Calcium and phosphate cannot leave, so their concentrations rise.
The ascending limb brings fluid back up to the cortex via the thick ascending limbs. It is these thick limbs that pump calcium out and preload the vascular bundles.
Little calcium leaves the ascending thin limbs, but urea and sodium chloride leave because extraction of water on the way down concentrated them inside the tubule lumens.
Although I drew them like a hairpin, the two limbs are separated each into its own micro – environment made by vessels and collecting ducts.
The Dream – Hypothesis
Being preloaded with calcium, the descending vas create high calcium concentrations in the capillaries that surround the thin limbs, and that higher concentration causes local supersaturation so plaque forms around the limbs.
In normal people the effect is relatively muted because delivery of calcium from the glomerulae down the descending thin limb and up the ascending thin limb to the thick ascending limbs is normal – not high.
In stone formers, urine calcium generally runs higher and that is in part due to greater delivery down the thin limb. So more calcium reaches the thick ascending limbs.
The thick limbs transport calcium via a charge difference across their walls, essentially via an electrical field, so more deliver transforms into more movement out into the space around the vascular bundles. This preloads them with more calcium than normal, and that raises local supersaturation in the capillaries around the thin limbs causing plaque. The greater delivery arises from reduced reabsorption of filtered calcium by the proximal tubule.
The Deduction
If this were true, then we must find more plaque forming on the ascending than the descending thin limb because water is leaving the latter without calcium and would dilute calcium delivered out of the surrounding capillaries.
‘Must’ is real here. Symmetry destroys the vas washdown hypothesis.
How can mere delivery of excess calcium cause plaque equally on both limbs when one is transferring water into the space surrounding it and the other is not?
No is No
If we do not find a large difference favoring plaque on the rising vas, the ascending vas, the theory is false and we move on.
The Stoller Hypothesis
Dr Marshall Stoller is a brilliant clinical scientists at UCSF. In fact, it was his original grainy pictures of plaque on human kidneys that started me on to plaque research. The latest paper from his group is a good place from which I can paraphrase his thinking.
Their Tissue Sample
Unlike our work, they used whole renal medullary papillary complexes harvested from kidneys removed because of cancer or other disease. So they had more tissue, a larger vision, from higher up, than us.
Their Proposed Mechanism for Plaque
Their key observation was that thin limbs higher up, nearer the cortex, formed mineral plugs. We would not have seen them. In their samples, interstitial crystals at the tip of the papillum – what we call plaque – was always accompanied by intra-tubular plugging higher up.
As the tubules narrow with descent, they propose, strains between the pressurized vas recta and the thin limbs will signal the interstitial cells to express bone genes and thereby mineralize the micro-environment.
Their Mechanism in Their Own Words
The best way to express their idea is to quote them:
‘Given that distal interstitial minerals were observed only in the presence of proximal intratubular biominerals, it is postulated that the architecture of the MPC (Figs 2-7) could link proximally distinct intratubular occlusion with distal interstitial mineralization via a mechanobiological switch located at the mid papillary interface. The mechanobiological switch can in turn stimulate distally located pericytes and other cells that can transdifferentiate into bone-like cells or express osteogenic matrix molecules resulting in distal interstitial mineralization (Figs. 8 and 9). Over time, the distal interstitial mineralization can emerge into the calyx, thus enabling the link between nephrocalcinosis (intratubular) and nephrolithiasis (kidney stone).‘ My bolding and italicising. MPC is short for medullary papillary complex.
In other words, to make plaque they propose osteogenic transformation. But unlike the Gambaro idea that arose in the context of medullary sponge kidney, here is a kind of mechanical effect from pressure differences triggering a cell response.
Their Necessary Prediction
This leads to the necessary prediction that one must find bone related genes associated with plaque. We could not, and therefore one critical test of this idea has falsified it. They also proposed ‘osteogenic matrix molecules’ might be expressed, a way around our failure to find bone cell genes. This leads to a test where one looks for those proteins.
The theory does not demand asymmetry of plaque formation between descending and ascending limbs as an inherent part of the mechanism. Likewise it could not explain asymmetry except to propose that the special proteins, if present, cluster there – on the rising not the falling side of the loop.
Why Has No One Proposed Dystrophic Calcification?
I know of no group actively pursuing this, though I may have missed it.
One reason, perhaps, is that papillary cells tolerate seemingly miserable conditions. They have little oxygen, high carbon dioxide concentrations, and are bathed by a fluid very high in sodium and potassium salts, and urea. I understand they have evolved for it, but like alley rats – also evolved in their way – they seem tough, nearly ineradicable.
Against papillary cell death is simple observation: One sees no obvious collections of cell debris in plaque deposits. So one immediate prediction is falsified already.
Even so, the idea is still viable, and perhaps justifies more attention.
The Test of Vas Washdown
An Illustration of What We Found
To let water out the descending thin limbs have aquaporin channels in their cell walls. The ascending limbs have none because they do not let water move through them. A potassium transporter with the catchy name of CLC-Ka is known to be absent on descending and present on ascending limbs.
Thus armed we – with massive difficulty – aimed to stain human papillary biopsies using antibodies to aquaporin and CLC-Ka and also stain for plaque using a third (Yasue) stain, asking if plaque localized with the one, the other, or both aquaporin and CLC-Ka.
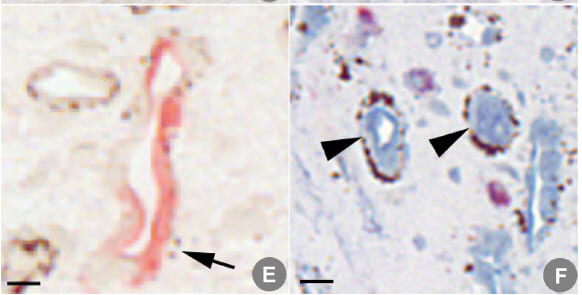
Here is a picture of what we found. Panel E shows a tubule stained with aquaporin; two tiny plaque particles are present at the arrow tip. Panel F shows CLC-Ka positive tubules ringed by masses of plaque.
No tubules had both aquaporin and CLC-Ka, as many other labs have reported.
A Sense of Numbers
In five separate patients, we stained all of the tubules in serial sections and photographed the entirety of those in a single field. Then, every tubule was graded as aquaporin positive or not, CLC-Ka positive or not, and plaque positive or not. No tubules were left ungraded, and each was numbered as the grade was taken to assure against double counting.
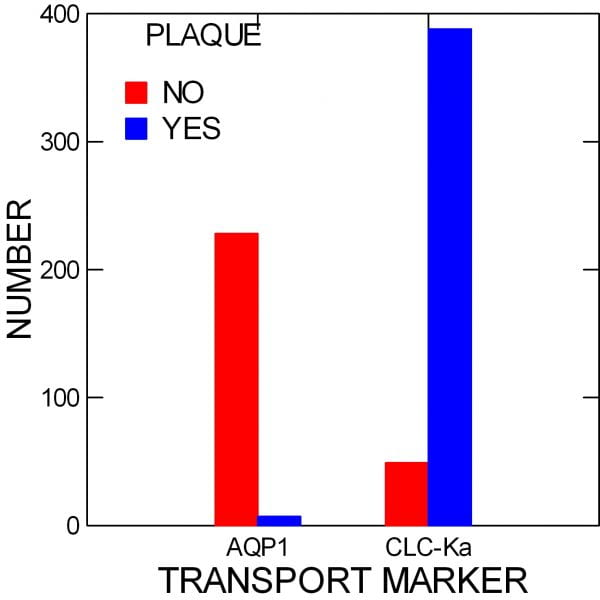 When we counted up all of the tubules, the asymmetry was astounding.
When we counted up all of the tubules, the asymmetry was astounding.
In those positive for Aquaporin (AQP1), the descending thin limbs, 228 had no plaque (red bar), vs, 7 with plaque (blue bar). For those positive for CLC-Ka, the ascending thin limbs, 49 had no plaque vs. 437 positive for plaque.
If you like statistics, the test for equal distributions of plaque between the two sides of the thin limbs gave a value of X2 = 464, p<0.001.
In other words, the chances of finding this kind of difference by chance alone are slim indeed.
What All This Means
The Data Are Probably True
Usually in science, measurements by professionals are accurate and others will find what we found if they measure as we measured. We expect others to repeat this work, as it is important, and probably after a bit of highly nuanced bickering about antibodies and tissue selection, things will be about as we report.
If not, then we measured wrong, the error will be corrected and the field move on.
Vas Washdown is Not As Yet False
We performed a critical test. The thin limb asymmetry arose out of the vas washdown theory as a necessary prediction. Bringing down an extra mote of calcium to increase local supersaturation, that small tilt of things, must work better when water is not flowing from inside the tubule to outside where plaque is forming. That is common sense. But here is a good moment to ponder ‘common sense’ in science.
How Much Water
In humans, how could we know? But in animals, micro-samples taken from where the thin limbs bend, the bottom of the hairpin, show about 1/2 the water that came in left through the walls of the descending limb. On the upside, about the same proportion of sodium and chloride leave, without water. So on the scale of size related to the actual loops, the water leaving on the downward side is about half of the flow they accommodate vs. none leaving on the upward side.
As for the flow, it is what the proximal tubule itself does not reabsorb, and we know that is perhaps 25% or 30% of what has been filtered out of blood. So 1/2 of 25 – 30% of filtrate leaves the descending thin limb. That is a lot for such a tiny segment.
How Much Extra Calcium?
We know the anatomy. The descending vessels must pass through what amounts to a tunnel made of thick ascending limbs that transport calcium out of their lumens without water. It is that calcium we propose fosters plaque when it gets down into the capillaries of the papillum near the ascending thin limbs.
The thick ascending limbs reabsorb about 15% of the calcium filtered, which is a lot compared to the percent in urine (2%). We have no real data at all showing that calcium actually gets down to the papillum, but the vessels are permeable to calcium. We have data showing that in stone formers with idiopathic hypercalciuria more filtered calcium is delivered out of the proximal tubule than normal, especially in men. Others have observed that large amounts of plaque tend to occur more in men than women (p=0.06).
Vas Washdown Does Not Contradict Presently Established Facts
As we made up the hypothesis we avoided ideas that established fact spoke against. This is usual in science. Why create a theory that has evidence against it on the books? But given some imagination and decent scholarship one can dream up all kinds of ways to explain how things like plaque might come to form.
The Asymmetry is a Novel Prediction
So a real test must predict something not already known, but more: Something one would not have specially looked for unless one had the theory in mind.
A valuable imagining should prompt one to make observations otherwise left undone, to obtain knowledge otherwise not sought because having no reason to suspect.
This is why imagination drives new science. It asks us to measure what we might never have chosen to measure. It specifies as important, as among whole lists of possible measurements, those few that test it to absolute, so that a failure leaves it to die without remorse.
What About Clinical Meaning
Vas Washdown
A lot.
Whatever reduces delivery to the thick ascending limb should reduce plaque. Thiazide does that, and so does low sodium diet. Whatever reduces interstitial papillary calcium concentration should reduce plaque. High fluid intake will do that by washing solute out of the tissues. These are two new necessary predictions of vas washdown. One may already have a fragment of support: A year of high fluids reduces the CT density of human papillae. Is this because plaque has diminished?
Be clear. These are required if the theory is to stay, but they lack the novelty and precision of the tubule asymmetry. All of these prediction concern factors that reduce stones altogether. By contrast the demand for ascending limb predominance is unique to the one hypothesis.
This is a crucial difference when one thinks about how science works, even if, as clinicians we might do the tests that have less of the unique and more of the pragmatic and beneficial about them.
The Stoller Hypothesis?
It leads to a renewed testing for bone genes and matrix protein co-localized with plaque. His dream demands that as a necessary deduction. Failure to find them destroys the idea. Finding them says the idea is not as yet wrong.
It is to this test some in the field should turn out of respect for an important possibility, and an important scientist.
More, bone transformation does not lead necessarily to the same clinical treatments for plaque prevention. It may require altogether different kinds of treatment not as yet obvious.
Dystrophic Calcification
If true it would push plaque prevention toward prevention of the presumed tiny areas of cell death, which would in turn aim attention at vascular disease or toxins as a cause. Given no serious research as yet, this possibility can only be mentioned in hope some will test it.
I wish to thank Dr John Asplin (Litholink Corp) for advice and careful reading of this article; he is my indispensable guide and critic.

Thanks for this fascinating research.
Thank you, Marvin. Have a good year. Fred
Hi Dr. Coe – I coach with Jill and she suggested I ask you the following: Can a Randall’s plaque disappear or resolve in some way? Early on in my kidney stone journey, the results of a CT scan mentioned a Randall’s plaque in my left kidney. My most recent CT results (after a bout with new-to-me uric acid stones) stated “no evidence of calculus” in my kidney and no mention of a Randall’s plaque any longer. Can a Randall’s plaque go away when better steps are taken with lower sodium/more water, or could they be dissolved like uric acid stones?
Hi Adrienne, Usually one cannot see plaque on CT, so I am not sure if it was there or disappeared. If you have uric acid stones, by all means treat them by raising urine pH. As for plaque, we do not know how it goes away. Regards, Fred Coe
Hi Dr. Coe – thank you for this information on the Randall’s plaque and my CT results. Yes I am being treated for the uric acid stones – Dr. Lin at Northwestern started me on potassium citrate in early November – first 15mg 2xday and then upped it to 20mg 2xday. I apparently now am an equal opportunity stoner – having made my initial calcium oxalate/calcium phosphate two years ago, and now these uric acid stones. They are all gone now out of my kidney (thankfully), and I am working with Jill again on prevention. Again, many thanks!
Hi Adrienne, Dr Lin is an excellent surgeon and also passionate about prevention. I know him and trust his judgement. Given calcium oxalate, calcium phosphate and uric acid, is it possible you have had chronic low urine volume? It is difficult to form all of these otherwise. Regards, Fred Coe
It was almost two years between my initial calcium oxalate/calcium phosphate stone and these two most recent uric acid stones. I know my urine volume was down during the time I made the uric acid stones and I’ve been working to get it back up to 3L/day (I’m at 2 1/2 – next week I should be back to 3). I had also been trying a high protein/low carb diet to help with weight loss . . . I think that backfired. Anyway, I had what I hope will be my last CT for a good long while this morning to make sure all the swelling is gone and that the forniceal rupture has healed. I see Dr. Lin again next week. There was talk that some of this could be hereditary (father died of kidney disease) and that allopurinol might be necessary, but blood work came back normal so I hope to avoid another med. I have one last question: Based on what I understood from reading the article you linked in your first response to me, dietary changes alone might not be enough to correct my pH issue. Is it possible that I would have to take potassium citrate forever?
Hi Adrienne, Given a large number of stones and diet changes such as you describe, treatment is complex. I would opt for the kidney stone diet – nothing else, and also adding chlorthalidone, because of so many stones. Likewise high fluids. But as I said, Dr Lin is very skilled at prevention, and this is merely an outsider commenting. It is up to him to stop the stones, and he is very good at it. Regards, Fred Coe
Dr. Coe – I’m looking for a good urologist in the Baltimore / Annapolis Maryland area? Can you recommend someone?
Dr Brian Matlage at Johns Hopkins is outstanding. He is a friend of mine, please feel free to say I mentioned him to you. Regards, Fred Coe
Thank you Dr. Coe!
Thank you doctor for the information
My mother in law is diagnosed with a 3mm lower pole kidney stone in the left side in the health check-up with no obstruction or pain can the kidney stones pass on their own or they need a surgery ?
Hi Jihitha, a non obstructing stone can be left alone. But she might want to find out why she formed it and take steps to prevent more. Regards, Fred Coe
Dr. Coe,
Thank you for this great synopsis of plaque theory. I am a curious urology resident who is interested in studying plaques. Do you have any thoughts on why we don’t observe plaques in mice or other animals? Lack of an animal model is certainly hindering this research. Would love to talk more.
Hi Daniel, Please feel free to email me directly so I can help you find a way. Coe@uchicago.edu. Regards, Fred